Prior Authorization Services That Reduce Administrative Burden
As a specialized prior authorization company, we manage the entire approval lifecycle, from intake and documentation to payer submission and follow-ups.

Prior Authorization Challenges Slowing Care, Cash Flow & Operations
Managing healthcare prior authorization internally often leads to delays, documentation gaps, and revenue risks that impact both patient access and financial performance.



What Makes Chirok Health a Trusted Prior Authorization Company
Chirok Health delivers structured, end-to-end prior authorization services built to handle payer complexity, documentation demands, and high approval volumes.
How We Differ?
- Approval Accuracy That Prevents Costly Rework
- Scalable Support Without Adding Internal Burden
- Faster Turnaround Across Complex Specialties

Authorization Specialists
Certified experts managing complex payer approvals end-to-end.

Process-Driven Execution
Standardized workflows ensure consistent authorization handling.

Prior Authorization Services Across FFS & VBC Models
Our prior auth services adapt to both fee-for-service volume demands and value-based care documentation rigor, ensuring compliant approvals, faster decisions, and reimbursement protection.

Fee-for-Service Authorization Management
In high-volume environments, we streamline healthcare prior authorization for imaging, procedures, and specialty services, reducing scheduling delays and preventing authorization-related denials.

Value-Based Care Authorization Support
As a specialized prior authorization company, we align submissions with medical necessity, care pathways, and payer quality requirements to support outcomes-driven reimbursement models.
Core Capabilities Powering Our Prior Authorization Services
Chirok Health delivers end-to-end prior auth services that combine intake precision, documentation coordination, payer communication, and status governance to ensure faster, compliant approvals.

Authorization Intake & Case Creation
Every request is logged, verified, and prioritized through structured workflows. Our teams initiate healthcare prior authorization cases with complete service, provider, and payer data accuracy.

Clinical Documentation Coordination
We collect, review, and organize medical records, treatment notes, and supporting documentation required for medical necessity validation before submission.

Payer Submission & Follow-Ups
As a specialized prior authorization company, we manage portal submissions, call-based authorizations, and proactive payer follow-ups to accelerate determinations.
Status Tracking & Authorization Governance
Our prior authorization services include real-time case monitoring, approval tracking, and escalation handling to ensure no request is delayed or missed.
How Our Prior Authorization Services Work
Chirok Health follows a structured, multi-stage prior authorization workflow that manages intake, documentation, payer submissions, and approval tracking with operational precision and compliance.
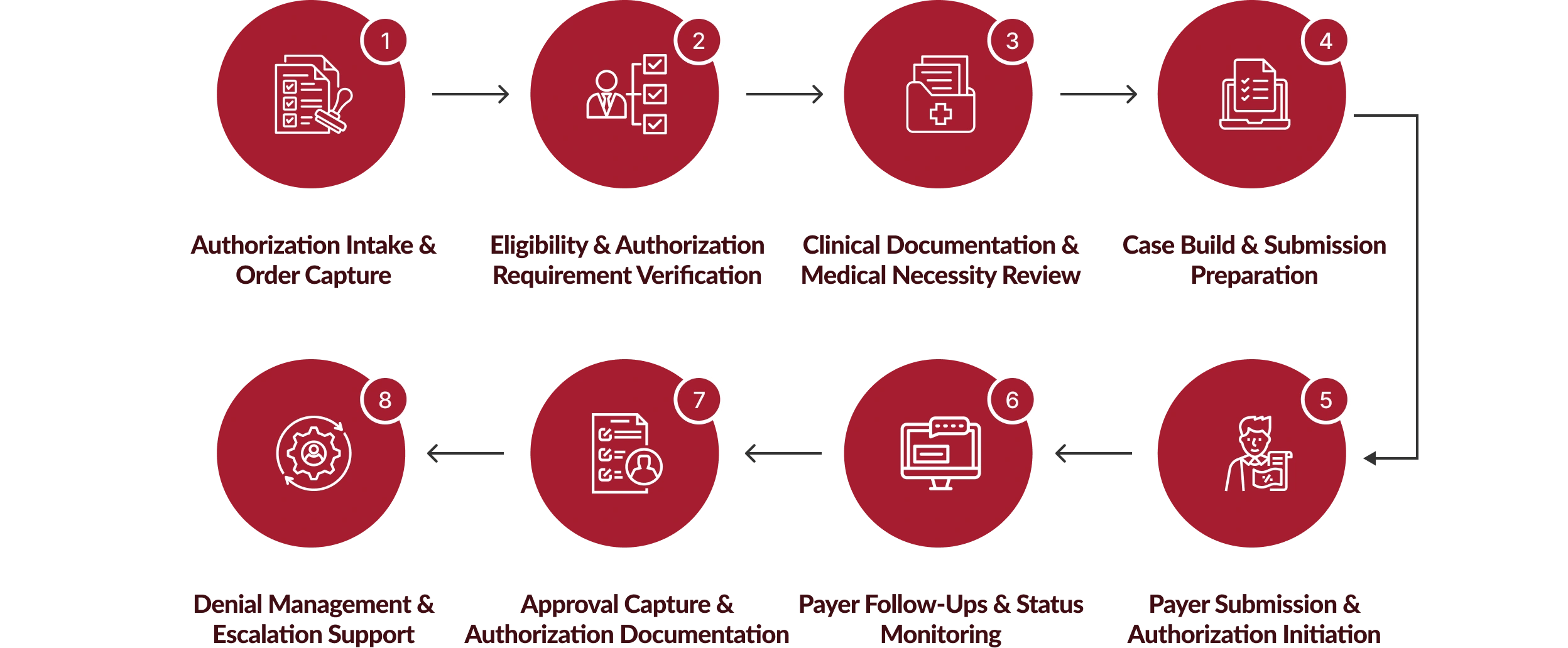
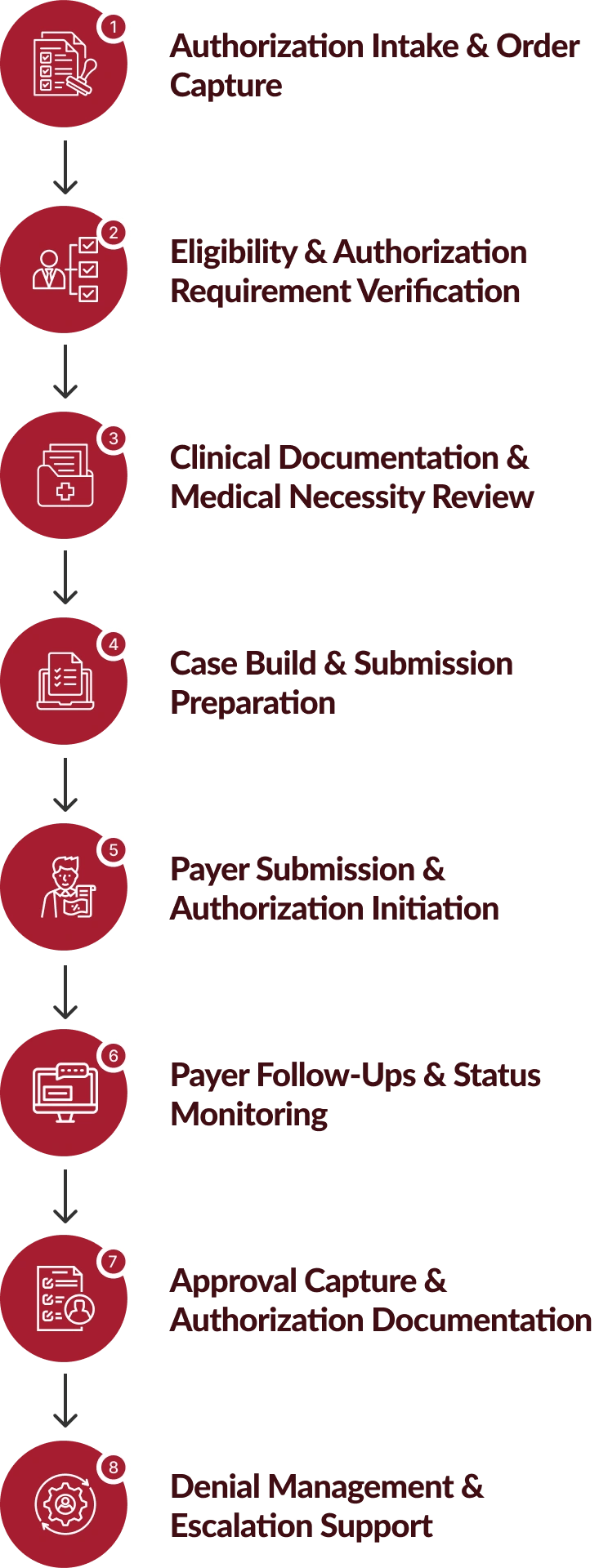
The Strategic Benefit of Partnering with Us For Prior Authorization Services
Drive faster approvals, reduce administrative strain, and strengthen reimbursement outcomes with expert-led prior auth services.

Structured workflows and proactive payer follow-ups help accelerate healthcare prior authorization decisions and reduce scheduling bottlenecks.
Our prior authorization company ensures complete documentation, coding alignment, and medical necessity validation before submission — minimizing preventable denials.
When you outsource prior authorization, internal teams spend less time on calls, portals, and paperwork.
Approvals secured in advance prevent treatment delays and last-minute cancellations.
Accurate prior authorization services protect high-value procedures from authorization-related write-offs.
Performance Metrics That Define Our Authorization Excellence
Our prior authorization services are engineered to improve approval velocity, documentation quality, and payer response outcomes, delivering measurable operational and financial performance gains.
EHR Expertise in Prior Authorization Services
Our prior authorization services operate directly within your existing EHR, enabling real-time case initiation, documentation access, and authorization tracking.
Why EHR Expertise Matters?
- Authorization requests initiated from scheduled encounters
- Immediate access to clinical documentation
- Real-time authorization status updates








Who we serve
We support healthcare organizations with specialized prior authorization services that streamline approvals, strengthen documentation alignment, and safeguard reimbursement across care settings.

Hospitals
Managing high authorization volumes across inpatient and outpatient services, we help hospitals secure timely approvals, prevent treatment delays, and reduce authorization-related denials.

Community & Integrated Health Systemss
Our prior auth services scale across multi-facility environments — standardizing workflows, improving payer coordination, and ensuring consistent approval management.

Academic Medical Centers
We support complex care environments by coordinating authorizations for specialized procedures, research-driven treatments, and teaching hospital workflows.

Medical Groups
From specialty referrals to diagnostic services, we streamline healthcare prior authorization requests while reducing administrative strain on clinic teams.

ACOs & Risk-Bearing Organizations
We align prior authorization processes with value-based care models, ensuring medical necessity documentation supports both approvals and risk performance.
Voices of the Organizations We Support
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Start Streamlining Your Prior Authorization Process Today
Whether you’re looking to outsource prior authorization, reduce submission delays, or improve payer response times, our experts are ready to design a workflow tailored to your organization’s needs.
Contact Form
Got Questions?
We’ve Got Answers!
Prior authorization services manage the process of obtaining payer approvals before medical services, procedures, or medications are delivered. These services include intake, eligibility checks, documentation collection, submission, payer follow-ups, and approval tracking to ensure treatments are authorized and reimbursable.
Organizations outsource prior authorization to reduce administrative workload, improve approval turnaround times, and minimize denial risk. An experienced prior authorization company manages payer communication, documentation requirements, and status tracking, allowing clinical and front-office teams to focus on patient care.
Comprehensive prior auth services typically cover request intake, insurance verification, medical necessity documentation, payer submission, follow-ups, approval capture, and denial escalation. This full lifecycle management ensures healthcare prior authorization requests are processed accurately and efficiently.
Prior authorization services prevent denials by validating medical necessity, confirming payer requirements, and ensuring documentation completeness before submission. Accurate approvals secured pre-service reduce retroactive denials and protect procedure reimbursement.
High-authorization specialties such as radiology, oncology, cardiology, orthopedics, behavioral health, and specialty pharmacy benefit significantly. These fields require frequent payer approvals, making outsourced prior authorization operationally and financially valuable.
A prior authorization company typically works within or alongside EHR platforms to access orders, clinical documentation, and scheduling data. This integration enables real-time request initiation, faster documentation retrieval, and streamlined authorization tracking.





















