Helping Organizations Fix Claim Edits and Rejections
Strengthen your clean claims process with proactive claim edits and rejections management. Chirok Health identifies billing edits early, accelerates corrections, and drives claim error prevention.

The Hidden Challenges Behind Claim Edits and Rejections
Disconnected workflows, front-end data gaps, and evolving payer rules make claim edits and rejections one of the biggest barriers to a predictable, clean claims process.



Why Healthcare Organizations Trust Our Claim Edits and Rejections Services?
Chirok Health combines deep revenue cycle expertise with structured claim rejection management workflows to resolve billing edits faster and strengthen your clean claims process.
Performance Drivers
- Early detection workflows reduce preventable claim error risks
- Dedicated teams resolve rejections without AR delays
- Continuous monitoring improves long-term billing accuracy

Clearinghouse & Payer Expertise
Aligned to payer rules and clearinghouse edits for accurate first-pass corrections.

Specialty-Aligned RCM Support
Claim edits and rejections workflows tailored to specialty billing needs.

Claim Edits and Rejections Support for FFS & VBC Models
Specialized claim rejection management workflows designed to protect revenue integrity across both fee-for-service and value-based reimbursement structures.

FFS Claim Accuracy
High-volume billing edits resolution to accelerate the clean claims process in fee-for-service environments.

VBC Revenue Integrity
Claim error prevention aligned to risk, quality metrics, and value-based reimbursement models.
Core Capabilities Powering Claim Edits and Rejections Excellence
Our claim edits and rejections framework combines automation, analytics, and expert review to streamline claim rejection management, resolve billing edits faster, and reinforce long-term claim error prevention.

Pre-Submission Edit Reviews
Advanced billing edits validation to catch errors before claims enter the payer workflow.

Rejection Resolution Workflows
Structured claim rejection management to correct and resubmit claims without delay.

Root Cause Analytics
Data-driven insights to identify patterns and strengthen claim error prevention strategies.

Clean Claims Optimization
Process enhancements designed to accelerate acceptance and improve clean claims process performance.
How We Resolve Claim Edits and Rejections at Scale?
Our workflow integrates automation, expert review, and payer-aligned validation to streamline claim rejection management, eliminate billing edits, and reinforce a high-performing clean claims process.
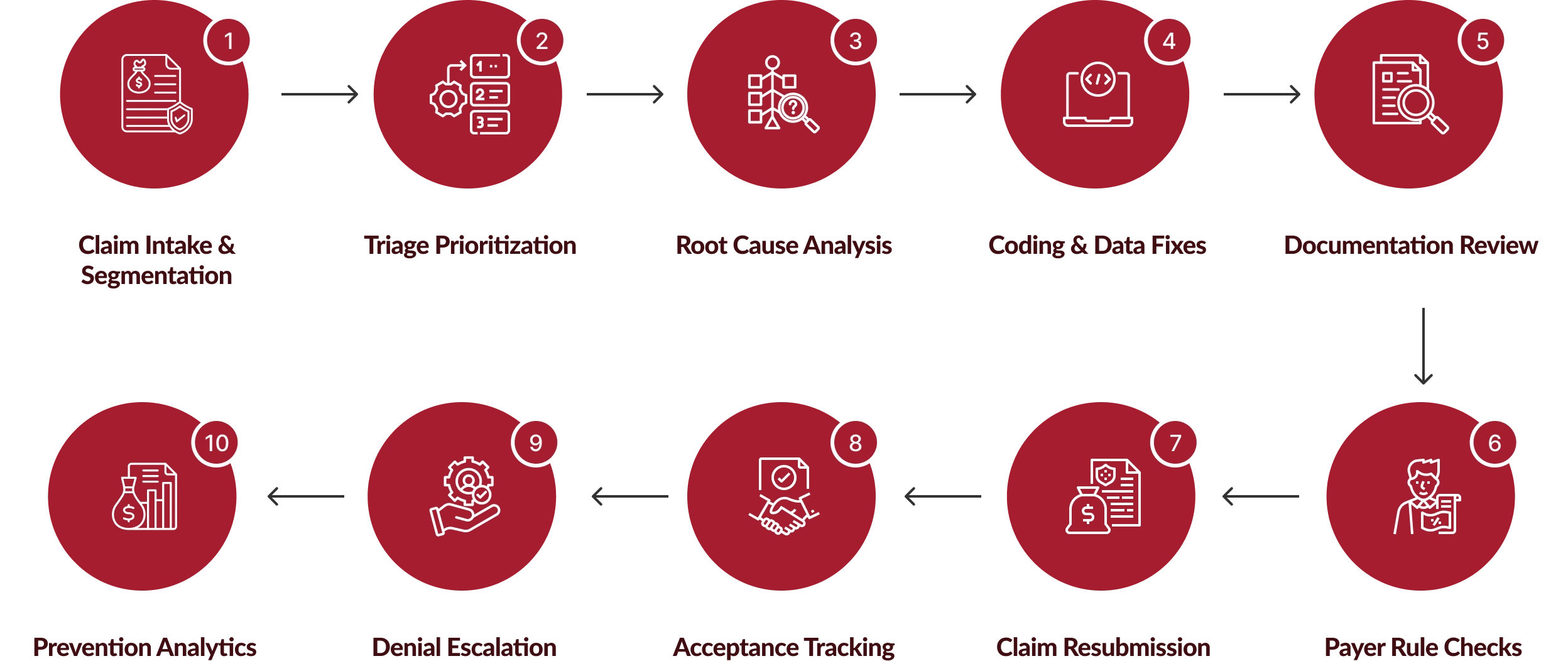
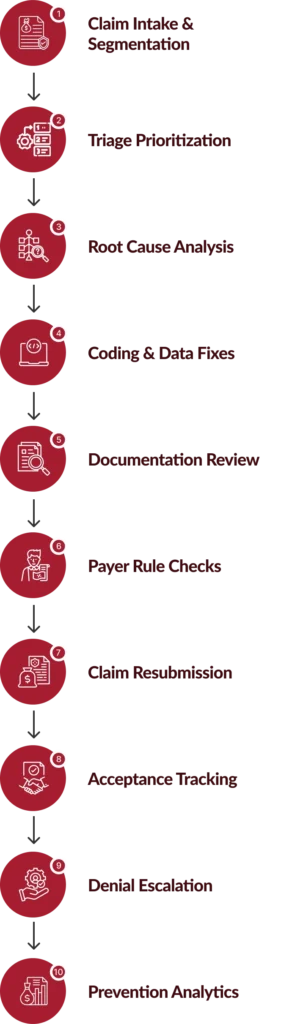
Benefits of Our Claim Edits and Rejections Services
Transform billing performance with structured claim rejection management and scalable claim error prevention strategies.

Our teams resolve billing edits before submission, reducing payer back-and-forth and improving first-pass claim acceptance across specialties and payers.
Focused claim rejection management workflows identify recurring payer triggers and eliminate preventable front-end submission errors.
Centralized tracking dashboards provide real-time insight into billing edits, correction timelines, and resubmission performance.
By shortening edit resolution cycles, organizations see quicker adjudication and improved cash flow predictability.
Root cause analytics help prevent repeat claim edits and rejections while strengthening long-term billing accuracy.
Performance Gains from Optimized Claim Edits and Rejections
Our claim edits and rejections framework delivers measurable financial and operational improvements, reducing billing edits, accelerating resubmissions, and strengthening enterprise-wide claim error prevention.
EHR Expertise for Claim Edits and Rejections Management
Our teams work within your EHR to identify billing edits, streamline claim rejection management, and support a stronger clean claims process.
Impact of EHR Expertise
- Real-time visibility into claim edits and rejections
- Faster correction cycles within existing workflows
- System-driven claim error prevention controls








Who we serve
Supporting healthcare organizations with specialized claim edits and rejections services that reduce billing edits, strengthen claim rejection management, and improve clean claims process performance.

Hospitals
Supporting real-time resolution of claim edits and rejections across inpatient and outpatient encounters to reduce reimbursement delays and downstream revenue loss.

Community & Integrated Health Systems
Delivering scalable claim rejection management across facilities to standardize correction workflows and strengthen system-wide clean claims process performance.

Academic Medical Centers
Addressing complex documentation and teaching physician billing structures with structured claim error prevention and edit resolution processes.

Medical Groups
Improving encounter-level billing accuracy by resolving claim edits and rejections quickly without disrupting provider documentation and coding workflows.

ACOs & Risk-Bearing Organizations
Ensuring accurate claim submission and correction workflows to support value-based reimbursement and risk-adjusted revenue performance.
Voices from Our Client Partnerships
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Start Strengthening Your Claim Edits and Rejections Performance
Partner with experts in claim rejection management and billing edits resolution to accelerate claim accuracy and reimbursement outcomes.
Contact Form
Got Questions?
We’ve Got Answers!
Claim edits and rejections occur when billing errors prevent a claim from moving forward for payer processing. Edits are system-flagged issues identified before submission or adjudication, while rejections happen when claims fail clearinghouse or payer validation checks. Effective claim edits and rejections management ensures errors are corrected quickly to maintain a smooth clean claims process.
A claim rejection happens before payer adjudication — meaning the claim was never processed for payment due to billing edits or data errors. A denial occurs after adjudication, when the payer reviews the claim but refuses reimbursement. Resolving rejections early is critical for claim error prevention and faster revenue recovery.
Unresolved billing edits and rejections delay claim submission, increase accounts receivable days, and create avoidable rework. Without structured claim rejection management, organizations risk timely filing issues, cash flow disruption, and downstream denials that impact overall financial performance.
Common claim rejection drivers include patient demographic inaccuracies, invalid or inactive insurance coverage, coding mismatches, missing modifiers, authorization gaps, and payer or provider ID errors. Structured claim edits and rejections services help identify these issues early and correct them before resubmission.
Preventing repeat billing edits requires root cause analytics, front-end workflow improvements, coding validation, and payer rule alignment. A structured claim error prevention strategy strengthens the clean claims process and reduces long-term rejection volumes.
Outsourcing provides access to specialized expertise, automation tools, and dedicated correction teams that accelerate resolution timelines. External partners help reduce billing edits, improve claim acceptance rates, and build scalable claim rejection management frameworks without increasing internal workload.





















