Denial Management Services for Healthcare Organizations
Prevent revenue loss with denial management services that combine expert claim denial management and intelligent workflows to recover payments faster.

The Growing Challenges Behind Healthcare Claim Denials
Rising payer scrutiny, coding changes, and documentation gaps are making claim denial management increasingly complex, driving payment delays and preventable revenue loss.



Why Healthcare Organizations Trust Our Denial Management Services?
Chirok Health combines payer expertise, analytics, and proven appeal frameworks to resolve denials faster, while strengthening long-term denial prevention.
The Impact on Your Revenue Cycle
- Faster turnaround on high-value denied claims
- Reduced repeat denials through root cause correction
- Stronger payer compliance and audit readiness

Specialized Denial Experts
Certified specialists resolving clinical and technical denials end-to-end.

Denial Management Specialists
Experts managing complex denials from review to recovery.

Denial Management Services for FFS and Value-Based Care Models
Different payment models demand different denial strategies. We tailor workflows, appeals, and analytics to optimize outcomes across FFS and VBC.

Denial Management for Fee-for-Service (FFS)
Our claim denial management approach accelerates resubmissions and maximizes per-claim revenue recovery.

Denial Management for Value-Based Care (VBC)
Our denial management specialists address documentation, risk adjustment, and medical necessity denials impacting quality-linked payments and shared savings performance.
Advanced Capabilities Behind Our Denial Management Services
Our denial management services combine analytics, clinical expertise, and automation to resolve denials faster and prevent recurrence.

Denial Identification & Classification
We analyze payer codes, CARCs, and RARCs to categorize denials accurately and prioritize high-impact recovery opportunities.

Root Cause & Trend Analysis
Advanced analytics uncover denial drivers across payers, providers, and service lines to strengthen denial management solutions.

Appeals & Resubmission Management
Our denial management specialists manage appeals, documentation, and corrected claims through every level of review.

Denial Prevention Strategies
We implement workflow edits, coding education, and compliance checks to reduce repeat claim denial management issues.
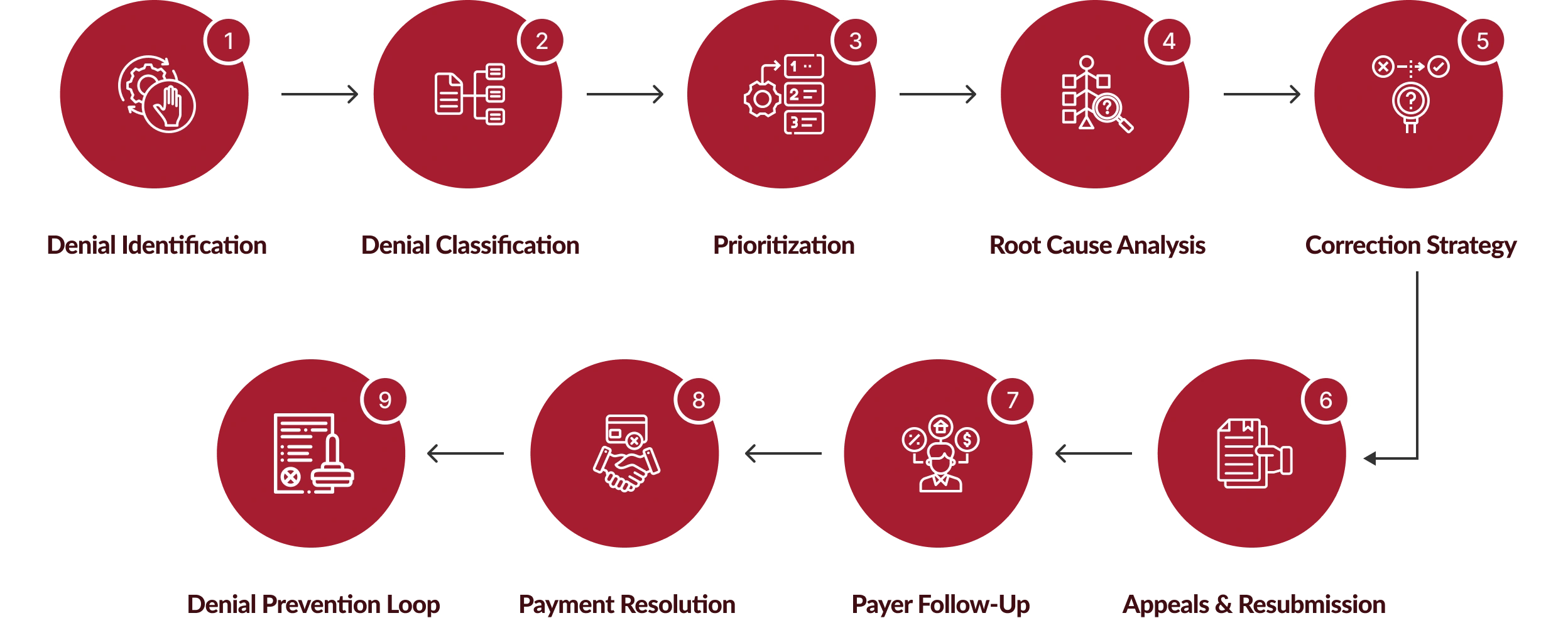
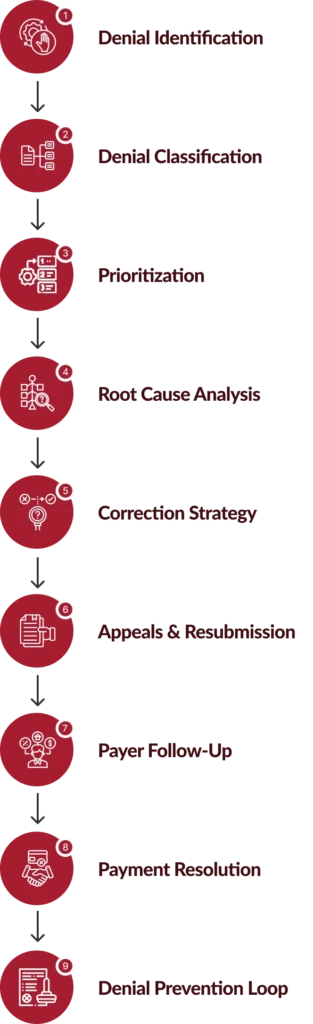
How Our Denial Management Services Work?
Chirok Health’s denial management services follow a structured, analytics-led workflow designed to recover revenue quickly while addressing the root causes of denials.
How Healthcare Organizations Benefit from Our Denial Management Services?
Our denial management services deliver more than recovery; they strengthen financial performance, operational efficiency, and payer alignment.

Our denial management specialists fast-track appeals, corrected claims, and payer follow-ups, reducing reimbursement delays and unlocking trapped revenue.
Root cause analysis and workflow corrections prevent repeat claim denial management issues across coding, authorization, and documentation.
Denial insights strengthen front-end edits and billing accuracy, increasing clean claim submission rates.
Our denial management solutions align submissions with evolving payer rules, minimizing audit risks and technical denials.
We offload denial tracking, appeals, and reporting, freeing internal teams to focus on higher-value RCM priorities.
Results That Define Our Claim Denial Management Performance
Our denial management services deliver measurable financial and operational improvements, from faster recovery timelines to reduced denial recurrence.
EHR Expertise in Denial Management Services
Our denial management staff works directly with your EHR to streamline workflows, improve data accuracy, and accelerate claim denial management resolution.
What This Enables
- Faster denial identification and work queues
- Reduced manual documentation gaps
- Real-time claim status visibility








Who we serve
Supporting healthcare organizations with specialized denial management services that reduce claim rejections, strengthen correction workflows, and improve clean claim performance across the revenue cycle.

Hospitals
Supporting real-time denial resolution across inpatient and outpatient claims to reduce reimbursement delays and downstream revenue loss.

Community & Integrated Health Systemss
Delivering scalable claim denial management across facilities to standardize corrections and strengthen system-wide reimbursement performance.

Academic Medical Centers
Addressing complex documentation and teaching physician billing structures with structured denial prevention and correction workflows.

Medical Groups
Improving encounter-level billing accuracy by resolving denials quickly without disrupting provider documentation and coding processes.

ACOs & Risk-Bearing Organizations
Ensuring accurate denial correction workflows that support value-based reimbursement and risk-adjusted revenue performance.
Client Experiences That Speak for Themselves
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Recover More Revenue With Expert Denial Management Services
Are you managing rising denial volumes or looking to prevent recurring claim losses? Our denial management services deliver the expertise, analytics, and workflows needed to improve financial performance.
Contact Form
Got Questions?
We’ve Got Answers!
Denial management services involve identifying, analyzing, correcting, and preventing denied insurance claims to recover lost revenue. These services include denial tracking, root cause analysis, appeals management, payer follow-ups, and prevention strategies designed to improve clean claim rates and reimbursement performance.
Claim denial management improves revenue cycle performance by accelerating appeals, recovering underpaid claims, and reducing repeat denials. By addressing documentation gaps, coding errors, and authorization issues, organizations can shorten AR days, improve cash flow, and strengthen first-pass claim acceptance rates.
A denial management specialist reviews denied claims, interprets payer denial codes, investigates root causes, prepares appeals, and manages resubmissions. They also collaborate with coding, billing, and clinical teams to correct systemic issues and prevent future denials.
The most common denial drivers include missing prior authorizations, eligibility errors, inaccurate patient data, coding discrepancies, insufficient documentation, medical necessity denials, and timely filing issues. Effective denial management services address each of these root causes systematically.
Denial management solutions use analytics, workflow edits, and compliance monitoring to identify denial trends and implement preventive controls. This includes front-end eligibility checks, coding audits, documentation improvement, and payer rule alignment to reduce recurring denials.
Outsourcing denial management services provides access to specialized expertise, scalable appeal resources, and advanced analytics without increasing internal workload. Many organizations outsource to improve recovery rates, reduce administrative burden, and accelerate denial resolution timelines.








