Revenue-Driven CPT, DRG & HCPCS Coding Optimization
Optimize financial outcomes with scalable DRG coding services, IP DRG coding, and CPT code accuracy programs designed to reduce denials, capture CC/MCCs, and improve case mix performance.

Challenges Where CPT Code Services & DRG Optimization Become Critical
Without proactive DRG coding and optimization and CPT code services, organizations face denials, underpayments, and audit vulnerability.



Why Chirok Health CPT, DRG & HCPCS Optimization Works?
Our specialists align documentation, coding, and reimbursement strategy to strengthen IP DRG coding, reduce denials, and improve case mix performance.
Why We Are Versatile:
- Documentation-driven DRG uplift strategies
- Modifier and charge capture optimization
- Concurrent coding intervention models

AHIMA/AAPC/ACDIS
Certified experts specializing in CPT and DRG coding optimization.

Specialty-Aligned Coding
Deep expertise across multi-specialty inpatient and outpatient coding.

Optimization Specifically for FFS & Value-Based Models
From IP DRG coding to outpatient CPT capture, we optimize coding workflows to support quality metrics, risk adjustment, and financial sustainability.

FFS Coding Optimization
Strengthen reimbursement through precise CPT code services and DRG coding services that improve charge capture, modifier accuracy, and inpatient payment integrity.

VBC Coding Optimization
Advanced In patient DRG coding and HCPCS optimization support risk adjustment accuracy, quality reporting, and value-based reimbursement alignment.
Core Components of CPT, DRG & HCPCS Optimization Services
We align clinical documentation, coding workflows, and compliance reviews to deliver scalable DRG coding and optimization across inpatient and outpatient care settings.

DRG Coding and Optimization
Advanced inpatient coding reviews improve DRG assignment accuracy, severity capture, and reimbursement performance.

CPT Code Services
Comprehensive CPT reviews ensure accurate procedure capture, modifier usage, and charge reconciliation across professional and outpatient billing.

In Patient DRG Coding
Specialized IP DRG coding audits identify missed CC/MCCs, documentation gaps, and sequencing errors impacting the case mix index.

HCPCS Optimization
We validate drugs, devices, infusions, and supply coding to eliminate revenue leakage and ensure compliant facility billing.
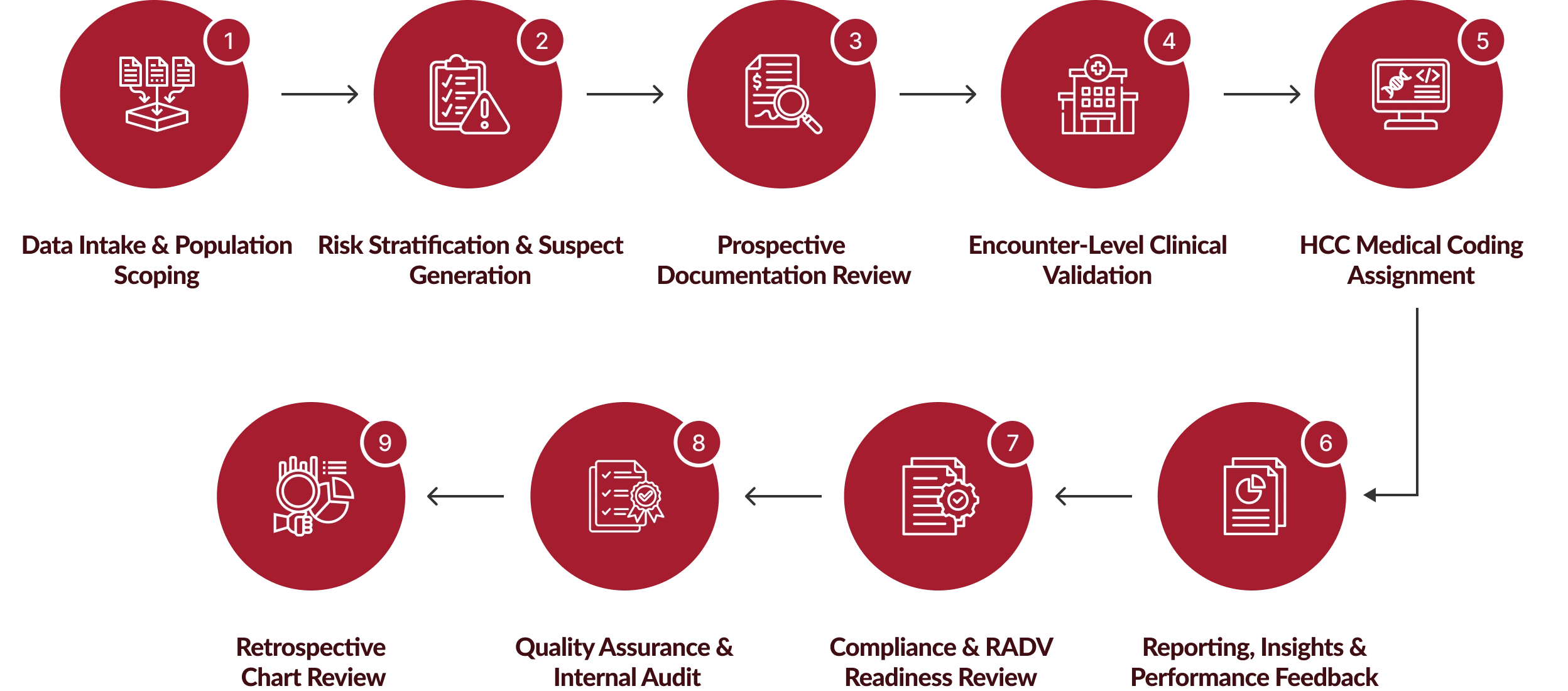
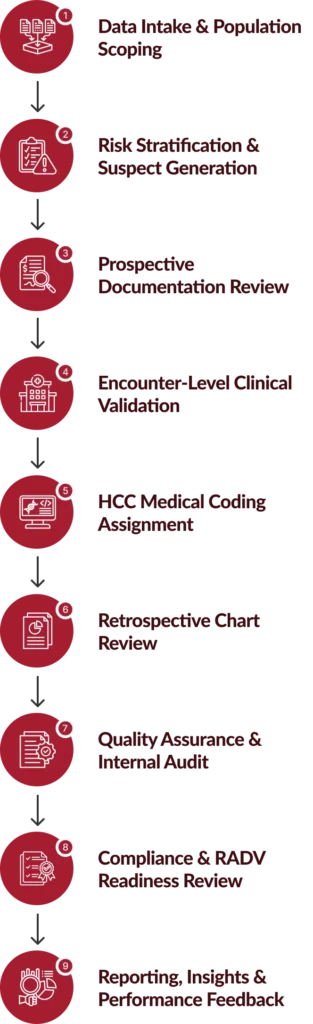
Our CPT, DRG & HCPCS Optimization Workflow
Our workflow integrates CPT code services, DRG coding services, In patient DRG coding, and HCPCS optimization to improve accuracy, reimbursement, and compliance.
Benefits of CPT, DRG & HCPCS Optimization Services
Unlock financial, operational, and compliance value through integrated CPT code services, DRG coding and optimization, and HCPCS accuracy programs.

Precise CPT code services and In Patient DRG coding ensure complete charge capture, accurate DRG assignment, and compliant HCPCS billing across care settings.
Proactive DRG coding services reviews eliminate coding discrepancies that trigger payer denials, clinical validation audits, and post-payment takebacks.
Advanced IP DRG coding analysis strengthens severity capture, CC/MCC reporting, and DRG weighting to improve inpatient financial outcomes.
We align clinical documentation with coding requirements to support compliant billing, quality reporting, and defensible reimbursement.
Integrated DRG coding and optimization streamlines inpatient and outpatient coding processes, improving turnaround time and operational efficiency.
Measurable Impact from CPT, DRG, & HCPCS Optimization
Our CPT code services, DRG coding and optimization, and HCPCS reviews deliver measurable reimbursement growth, denial reduction, and inpatient coding performance improvement.
Optimization That Works with Your Existing EHR
CPT code, DRG coding services, and HCPCS optimization are delivered within your EHR to drive coding accuracy and revenue integrity.
Why EHR Expertise Matters:
- Rapid EHR deployment accelerates coding optimization adoption.
- We work within your existing documentation and coding workflows.
- EHR-aligned reviews strengthen reporting, validation, and compliance.









Who we serve
Supporting healthcare organizations with CPT code services, DRG coding and optimization, and HCPCS expertise that improve documentation accuracy, reimbursement outcomes, and coding compliance at scale.

Hospitals
Supporting inpatient and outpatient coding accuracy through Inpatient DRG coding and CPT optimization to reduce DNFB, denials, and post-discharge rework.

Community & Integrated Health Systems
Delivering scalable DRG coding services across facilities to standardize documentation, improve coding consistency, and protect system-wide revenue.

Academic Medical Centers
Balancing complex care delivery and compliance requirements with advanced DRG coding and optimization during high-acuity inpatient encounters.

Medical Groups
Improving E/M accuracy and procedure capture through expert-led CPT code services that support providers without disrupting clinic workflows.

ACOs & Risk-Bearing Organizations
Ensuring accurate capture of risk-adjustable diagnoses through precise IP DRG coding and documentation optimization.
Hear from Healthcare Leaders We’ve Helped
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Start Optimizing Your CPT & DRG Coding Performance
Partner with Chirok Health to implement scalable CPT Code Services, DRG Coding Services, In Patient DRG Coding, and HCPCS optimization programs tailored to your organization’s revenue cycle goals, compliance priorities, and operational workflows.
Contact Form
Got Questions?
We’ve Got Answers!
CPT and DRG optimization services improve revenue by identifying undercoded procedures, missed CC/MCC conditions, and incorrect DRG assignments. This ensures accurate reimbursement, strengthens case mix index, and reduces revenue leakage across inpatient and outpatient encounters.
Organizations outsourcing DRG Coding Services typically see improved coding accuracy, denial reduction, higher CMI, compliant documentation, and faster coding turnaround times — all contributing to stronger financial performance.
In Patient DRG Coding reviews validate diagnosis sequencing, clinical specificity, and severity capture before billing. This prevents clinical validation denials, DRG downgrades, and post-payment audit exposure.
Yes. Optimization programs are embedded within existing EHR systems, allowing coders and auditors to review documentation, validate codes, and improve charge capture without disrupting clinical or billing workflows.
DRG Coding and Optimization strengthens risk-adjusted documentation, severity capture, and quality reporting accuracy, all of which directly impact performance and reimbursement under value-based care contracts.
Hospitals, health systems, academic medical centers, medical groups, and risk-bearing entities benefit most, as they manage complex documentation, inpatient coding volume, and reimbursement risk tied to CPT and DRG accuracy.





