AHIP - Medicare, Medicaid, Duals & Commercial Markets Forum (MMDC26)

Documentation Precision Is a Risk Strategy.
At AHIP 2026, Chirok Health is looking forward to sharing and gaining insight with Medicare Advantage plans, integrated health systems, and value-based organizations looking to reduce documentation volatility, strengthen audit defensibility, and align clinical and administrative workflows across hybrid payment models.
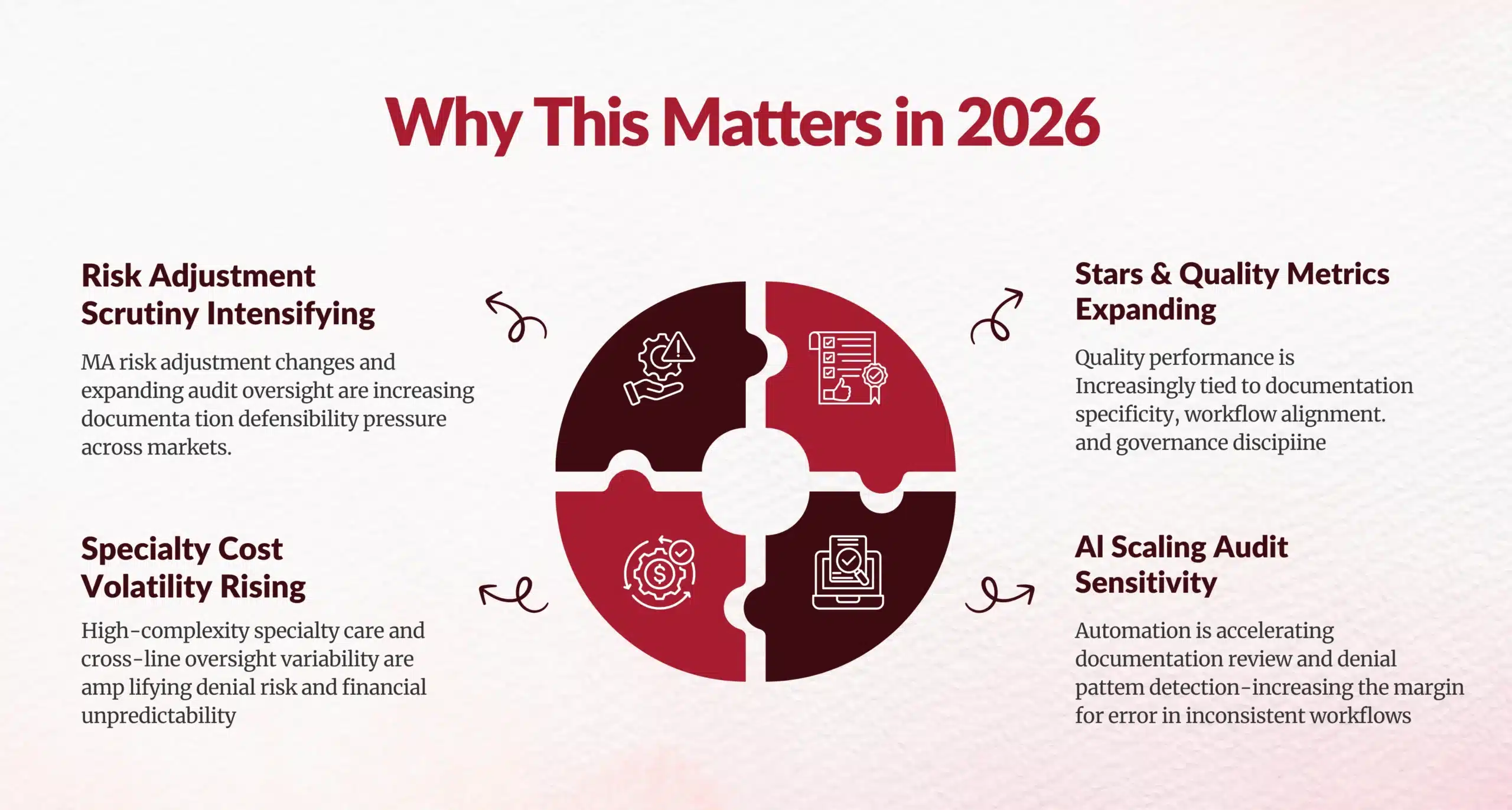
In 2026, quality performance, risk adjustment, and financial stability are operational disciplines not reporting functions.
Looking forward to continuing the conversation with you at AHIP.
30-Minute Executive Review

Meet Our Expert
Connect with Chirok Health leadership specializing in coding strategy, documentation integrity, and risk adjustment performance across complex payer programs.
What You’ll Gain
- Strategies to improve risk adjustment accuracy without aggressive coding practices
- Payment integrity frameworks that reduce provider abrasion
- Upstream documentation interventions that prevent downstream denials
- Audit readiness insights across MA, Medicaid, and dual populations
- Visibility into regulatory and compliance risk exposure
- Vendor-neutral perspectives on plan–provider performance alignment
Let’s Talk
If you’re focused on strengthening program performance while maintaining compliance and provider collaboration, we’d welcome the conversation.
Meet with Chirok Health at AHIP MMDC26 to explore how documentation accuracy, coding integrity, and upstream prevention strategies can support payment integrity, without disruptive operational change.
Ask about our accuracy-first performance assessment designed to highlight documentation risk, audit exposure, and denial vulnerability across your network.






