Inpatient Outpatient Coding Services for High-Volume Healthcare Organizations
Chirok Health delivers specialized inpatient medical coding and outpatient medical coding services aligned with payer rules, DRG/APC accuracy, and CDI best practices.

Coding Challenges That Emerge as Inpatient and Outpatient Volumes Grow
Inpatient outpatient coding becomes increasingly complex as volumes rise, regulations change, and documentation gaps persist, putting revenue, compliance, and reporting accuracy at risk.



What Makes Chirok Health’s Inpatient Outpatient Coding Reliable
Chirok Health applies certified expertise, specialty-aligned workflows, and built-in quality controls to deliver dependable inpatient outpatient coding across complex care settings.
Why We are Different:
- Specialty-aligned coding minimizes variation in inpatient and outpatient coding.
- Multi-level quality checks validate DRG, APC, and modifier accuracy
- Coding decisions align with payer rules and regulatory requirements.

Certified Clinical Coders
AHIMA, AAPC & ACDIS certified professionals

Specialty-Focused Coverage
Supporting 30+ healthcare specialties

Inpatient & Outpatient Coding Across Payment Models
Inpatient outpatient coding services structured to support accurate reimbursement, quality reporting, and risk performance across payment models.

Fee-for-Service Coding
Accurate inpatient and outpatient coding focused on DRG, APC, modifier use, and medical necessity to support compliant reimbursement.

Value-Based Care Coding
Coding that supports risk adjustment, quality measures, and complete clinical capture across inpatient and outpatient encounters.
Core Components of Our Inpatient Outpatient Coding Services
Chirok Health’s inpatient outpatient coding service covers the full coding lifecycle, from documentation review to final code assignment, across inpatient and outpatient settings.

Clinical Documentation Review
Review of provider documentation to support accurate diagnosis and procedure coding across inpatient and outpatient encounters.

Inpatient Coding (ICD-10-CM/PCS)
ICD-10-CM and ICD-10-PCS coding aligned to DRG logic, severity capture, and inpatient reimbursement requirements.

Outpatient Coding (CPT/HCPCS)
CPT and HCPCS coding with correct modifier use to support APC assignment and compliant outpatient billing.

Coding Quality Validation
Multi-level quality checks to validate code accuracy, consistency, and compliance before claim submission.
How Our Inpatient Outpatient Coding Services Process Works
Chirok Health follows a structured inpatient outpatient coding workflow that ensures documentation accuracy, compliant code assignment, and quality validation before claims move forward.
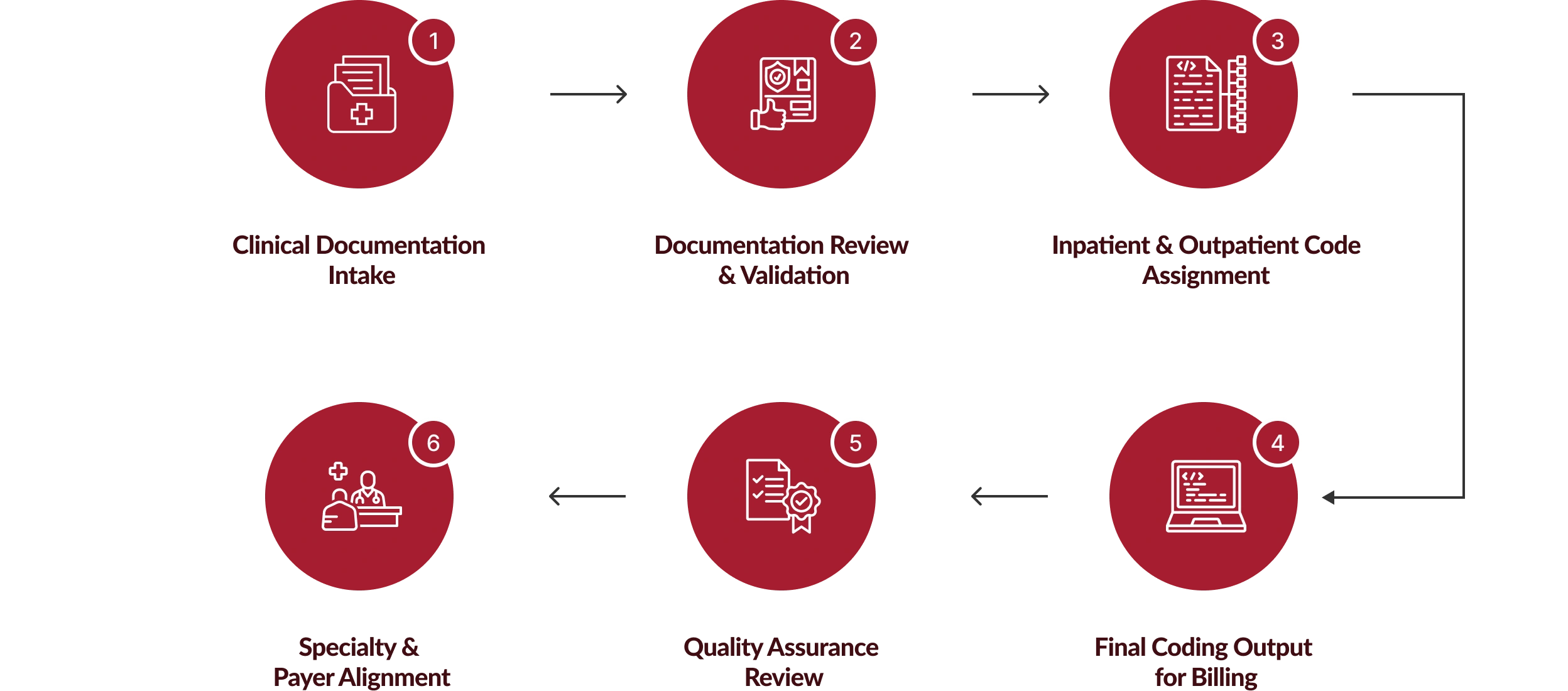
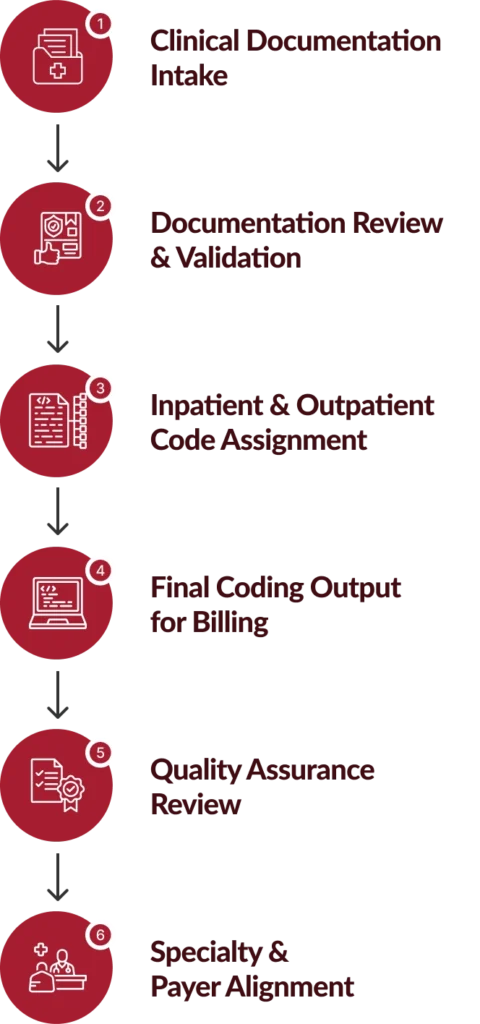
What Organizations Gain from Our Inpatient Outpatient Coding Services
Chirok Health’s inpatient outpatient coding services deliver measurable improvements across accuracy, compliance, reimbursement, and reporting.

Improved accuracy across inpatient and outpatient encounters reduces rework and downstream corrections.ent coding ensures patient complexity is fully and accurately reflected.
Consistent code assignment supports compliant reimbursement under fee-for-service and value-based care.
Complete clinical capture improves DRG severity, APC assignment, and quality reporting outcomes.ive reviews improve continuity and accuracy of chronic condition capture.
Alignment with payer rules and coding guidelines reduces denial and audit risk.ports equitable benchmarking, shared savings, and performance-based payments.
Reliable coding output supports cleaner billing, analytics, and revenue cycle decision-making.ms without increasing internal staffing or operational burden
Measured Outcomes from Expert Inpatient Outpatient Coding
Our inpatient outpatient coding services deliver consistent, measurable improvements in accuracy, turnaround time, and reimbursement performance across complex care settings.
Our Coders Work Directly Inside Your EHR
Chirok Health delivers inpatient outpatient coding services directly within your EHR, without parallel systems or manual workarounds.
Why EHR Adaptability Matters:
- Faster onboarding with minimal system setup
- Fewer workflow disruptions for clinical teams
- Accurate, system-native coding and reporting








Who we serve
Chirok Health supports healthcare organizations that rely on accurate inpatient and outpatient coding to strengthen reimbursement, compliance, and operational performance.

Hospitals & Health Systems
Supporting accurate inpatient medical coding and outpatient medical coding to improve DRG integrity, APC assignment, and audit readiness at scale.

Outpatient Care Organizations
Delivering consistent outpatient coding across clinics, EDs, and ambulatory settings without compromising accuracy or turnaround time.

Academic Medical Centers
Managing complex, high-acuity inpatient and outpatient encounters with clinically validated coding that supports teaching environments and compliance.

Medical Groups & Physician Practices
Improving documentation alignment and code accuracy across specialties to support compliant billing and reliable revenue performance.

ACOs & Risk-Bearing Organizations
Ensuring accurate inpatient and outpatient code capture to support quality reporting, financial performance, and value-based contract requirements.
Value-Based Care RCM Staff Augmentation
Dedicated Chirok Health specialists extend your value-based care revenue cycle, supporting risk, quality, and contract performance across your organization.
Hear from Organizations We’ve Helped
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Let’s optimize inpatient and outpatient coding accuracy and performance.
Whether you manage inpatient or outpatient coding at scale, Chirok Health helps improve accuracy, compliance, and turnaround time. Start a conversation for a tailored coding solution.
Contact Form
Got Questions?
We’ve Got Answers!
Medicare Advantage plans struggle with incomplete HCC capture from inconsistent documentation, impacting RAF scores and revenue. Chirok Health's certified coders ensure 23% RAF uplift through comprehensive chart reviews and prospective coding.
We deliver ICD-10-CM coding aligned with CMS guidelines, multi-level QA, and EHR-native workflows to maximize risk adjustment while minimizing audits. Schedule a RAF optimization consult.
ACOs need complete severity capture across inpatient/outpatient encounters for quality measures and shared savings. Our specialty-aligned coding boosts RAF scores 23% and supports HCC/quality reporting.
Full coverage for MSSP, Next Gen, and global risk models with accurate risk adjustment, DRG/APC validation, and payer-specific compliance.
Yes—our AHIMA/AAPC certified team manages 25% E/M volume increases with 99% accuracy, DRG integrity, and modifier expertise across 30+ specialties. Direct EHR integration eliminates backlogs.
EHR-native setup enables fast onboarding (days, not weeks) with minimal disruption, supporting hospitals, EDs, and clinics at scale.
Multi-level quality checks align with AHIMA, AAPC, ACDIS standards and payer rules, reducing denial exposure by validating DRG/APC/modifiers pre-submission. 99% accuracy proven.
Clients achieve 26% wRVU growth, 25% E/M volume increase, 23% RAF uplift, and cleaner revenue cycles. Finance leaders gain reliable billing insights
Our scalable team of certified experts eliminates hiring/retention issues, delivering consistent quality without backlogs or rushed coding.








