Concurrent Review for Risk-Bearing Organizations
Improve reimbursement with concurrent review, concurrent review, and retrospective chart review. Our clinical documentation review enhances RAF accuracy and lowers denials.

Clinical Documentation Gaps That Impact Revenue
Incomplete documentation, missed diagnoses, and delayed reviews weaken reimbursement accuracy. Without structured clinical documentation review, organizations face RAF erosion, denial risk, and compliance exposure.



Why Chirok Health’s Concurrent Review Works?
Our concurrent review model integrates clinical expertise with structured clinical documentation review to close gaps during active encounters.
The Strategic Advantage
- Real-time documentation correction reduces preventable denials.
- Clinical validation strengthens RAF and risk adjustment accuracy.
- Escalation workflows prevent post-discharge revenue loss.

Real-Time Clinical Oversight
Intervene before documentation gaps become denials.

Integrated CDI Review Framework
Aligned with concurrent and retrospective workflows.

Clinical Documentation Review for FFS and VBC Models
Our clinical documentation review services adapt to both fee-for-service and value-based care models, ensuring accurate reimbursement, compliant documentation, and optimized risk capture.

Clinical Documentation Review for FFS
Improve claim accuracy through structured concurrent review and retrospective chart review that reduce denials, correct coding gaps, and support compliant reimbursement.

Clinical Documentation Review for VBC
Enhance RAF accuracy and risk adjustment performance through concurrent review, retrospective chart review, and condition capture validation.
Core Capabilities of Our Concurrent Review Services
We combine clinical insight, coding precision, and audit-ready documentation strategies to improve financial integrity across payment models.

Prospective Chart Review
Identify documentation gaps before encounters are finalized, ensuring accurate diagnosis capture and compliant coding alignment.

Concurrent Review Oversight
Conduct real-time concurrent review to validate medical necessity, strengthen documentation clarity, and reduce preventable denials.

Retrospective Chart Review
Perform deep retrospective chart review to uncover missed conditions, coding inconsistencies, and RAF-impacting documentation gaps.

Enterprise CDI Review Framework
Deploy structured CDI review programs that align physicians, coders, and compliance teams under standardized documentation protocols.
Our Clinical Documentation Review Process
Our structured clinical documentation review methodology ensures documentation accuracy, compliance alignment, and financial performance optimization.
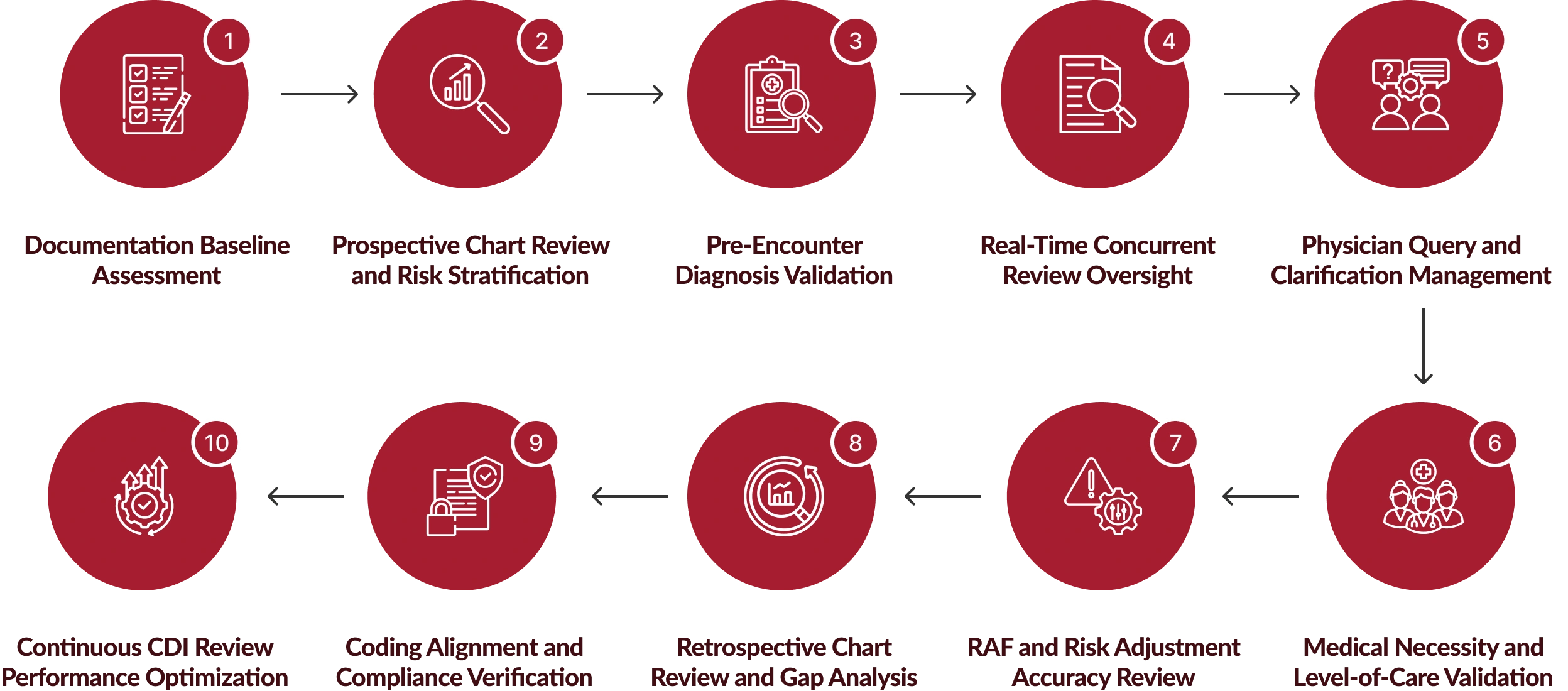
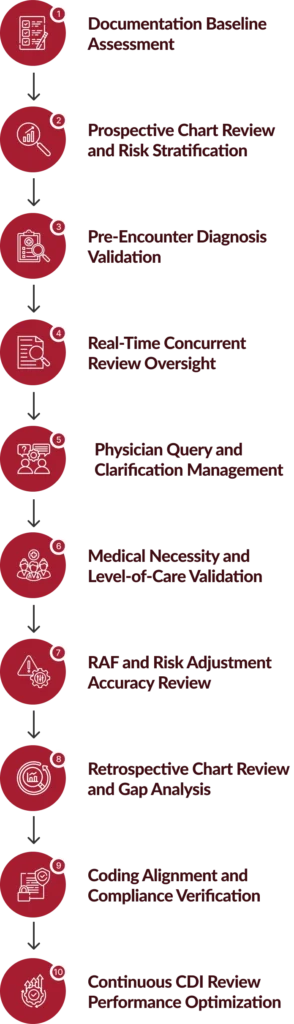
Benefits of Our Clinical Documentation Review Services
Our clinical documentation review improves reimbursement accuracy, strengthens compliance, and enhances risk adjustment performance across FFS and value-based care models.

Accurate chart notes ensure payments fully reflect the complexity of care delivered, supported by structured clinical documentation review and CDI review oversight.
A unified process integrates prospective chart review, concurrent review, and retrospective chart review to support both value-based care and fee-for-service requirements.
Comprehensive documentation validation aligned with payer-specific medical policies improves coding specificity and reduces preventable denials.
Embedded risk adjustment reviews protect RAF accuracy, ensuring FFS claim edits do not override clinically supported diagnostic information.
Scale your clinical documentation review program without the burden of staffing, training, or compliance management while meeting regulatory standards.
Tangible Results of Clinical Documentation Review
By integrating CDI review into every stage of the care lifecycle, we help organizations strengthen risk adjustment accuracy, reduce compliance exposure, and protect long-term revenue integrity.
Seamless EHR Alignment for Clinical Documentation Review
We align documentation oversight with your existing EHR infrastructure to strengthen coding accuracy, risk adjustment performance, and compliance readiness.
Operational Advantages
- Stronger alignment between documentation and coding
- Reduced rework from incomplete chart entries
- Real-time visibility into documentation gaps








Who we serve
Our concurrent review services improve documentation integrity, reimbursement accuracy, and risk adjustment performance across various healthcare organizations.

Hospitals
Strengthening inpatient and outpatient documentation through concurrent review and CDI review programs that reduce denials and improve reimbursement accuracy.

Community & Integrated Health Systems
Delivering scalable clinical documentation review across multiple facilities to standardize workflows and improve system-wide RAF and coding alignment.

Academic Medical Centers
Supporting complex documentation environments with structured prospective chart review and retrospective chart review processes that enhance compliance and audit readiness.

Medical Groups
Improving encounter-level documentation accuracy without disrupting provider workflows through embedded CDI review and real-time documentation oversight.

ACOs & Risk-Bearing Organizations
Enhancing risk adjustment accuracy and value-based reimbursement performance through integrated clinical documentation review strategies.
Trusted by Leading Healthcare Organizations
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Let’s Optimize Your Clinical Documentation Performance
Whether you are optimizing fee-for-service reimbursement or strengthening value-based performance, our clinical documentation review framework delivers measurable, compliant results.
Contact Form
Got Questions?
We’ve Got Answers!
Clinical documentation review is the structured evaluation of medical records to ensure diagnoses, procedures, and clinical details are accurately documented and supported. It improves reimbursement accuracy, strengthens compliance, and enhances risk adjustment performance across fee-for-service (FFS) and value-based care (VBC) models.
CDI review improves reimbursement by validating diagnosis specificity, confirming medical necessity, and aligning documentation with coding standards. By correcting documentation gaps before claim submission, organizations reduce denials and ensure payments reflect the true complexity of care delivered.
Concurrent review occurs during the patient encounter to address documentation gaps in real time, reducing preventable denials. Retrospective chart review takes place after discharge to identify missed diagnoses, coding inconsistencies, and risk adjustment discrepancies for reconciliation and improvement.
Prospective chart review evaluates documentation before claims are finalized. It identifies missing diagnoses, incomplete documentation, and risk capture gaps early, helping organizations protect reimbursement, improve compliance, and strengthen RAF accuracy.
Clinical documentation review ensures chronic conditions and comorbidities are fully documented and supported. Through structured CDI review, concurrent review, and retrospective chart review, organizations improve RAF accuracy and align documentation with CMS risk adjustment models.
Hospitals, medical groups, academic medical centers, and risk-bearing organizations benefit from clinical documentation review. These services reduce denials, improve coding specificity, strengthen compliance readiness, and optimize reimbursement across FFS and value-based care environments.

























