Claim Appeals & Payer Correspondence Made Seamless
Streamline denial appeals, medical appeals, and payer correspondence with expert-led workflows that accelerate overturns, reduce AR aging, and protect earned reimbursement.

Claim Appeals & Payer Correspondence Challenges Organizations Face
As denial volumes grow, inefficient payer correspondence and documentation shortfalls create costly delays. Without optimized claim appeals strategies, revenue recovery remains limited.



What Makes Our Claim Appeals Approach Different?
Chirok Health combines structured claim appeals workflows, clinical-backed medical appeals, and streamlined payer correspondence to accelerate overturns while reducing operational burden.
Designed for Appeals Success:
- Specialized denial appeals expertise improves overturn rates.
- Structured payer correspondence reduces response delays.
- Clinically validated medical appeals strengthen payer decisions.

Denial Appeals Experts
Specialists managing complex denial appeals end to end.

Payer Response Management
Streamlining payer correspondence workflows.

Appeals & Correspondence for FFS and VBC Models
Tailored denial appeals and medical appeals strategies designed to perform across FFS billing and value-based care contracts.

FFS Appeals Management
High-volume claim appeals and denial appeals support to recover underpaid and denied fee-for-service claims faster.

VBC Denial Appeals
Specialized medical appeals and payer correspondence for risk-adjusted and value-based reimbursement models.
Core Capabilities Of Our Claim Correspondence and Appeals Success
We unify claim appeals, payer correspondence, and documentation-driven medical appeals into a scalable model built for denial reduction and revenue protection.

Claim Appeals Management
Comprehensive claim appeals handling from denial review through submission, tracking, and payer resolution.

Denial Appeals Resolution
Focused denial appeals strategies addressing coding, authorization, and medical necessity denials.

Payer Correspondence Management
Managing payer correspondence across portals, fax, and email to ensure timely responses and appeal progression.

Documentation-Led Appeals
Clinically validated medical appeals built on documentation, coding accuracy, and payer policy alignment.
How We Manage Claim Appeals From Intake to Overturn?
Each denial appeals case follows a standardized workflow designed to strengthen medical appeals and improve overturn rates.
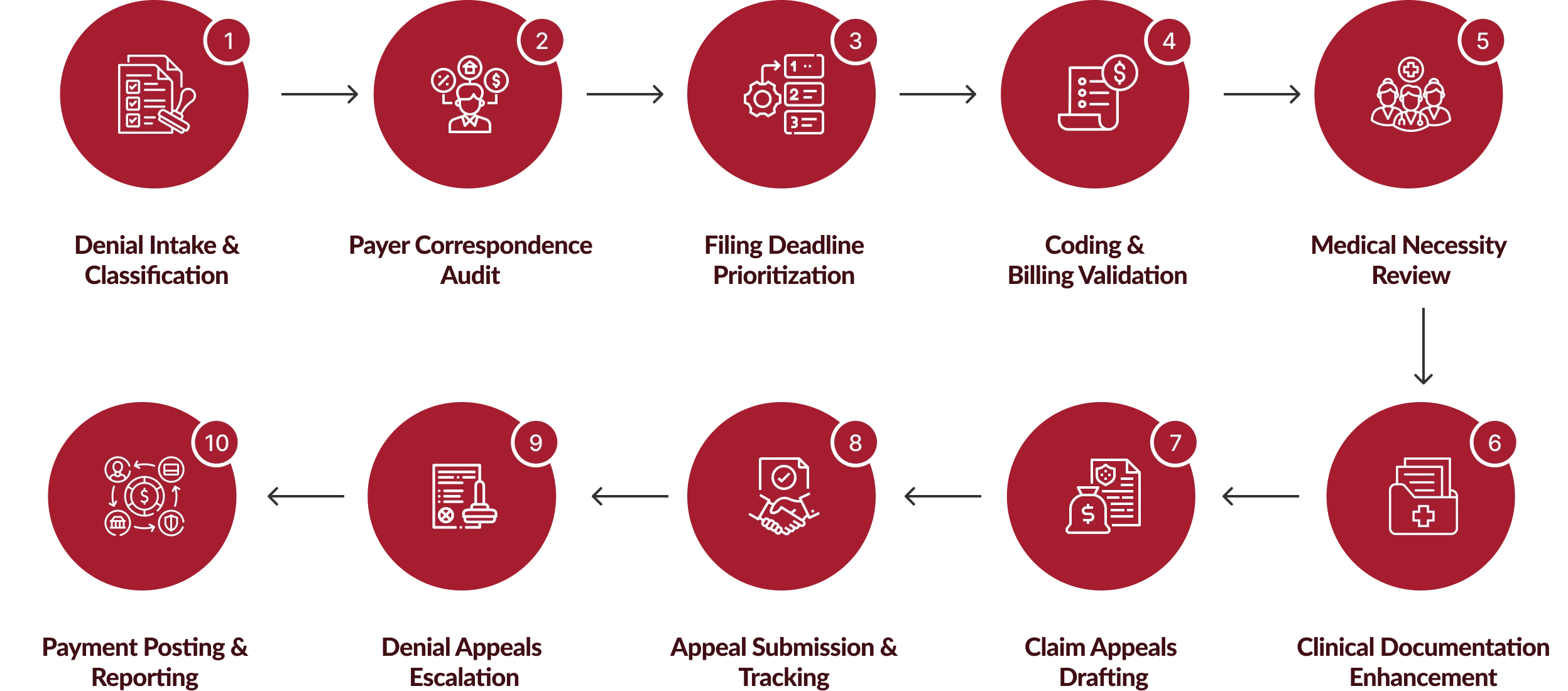
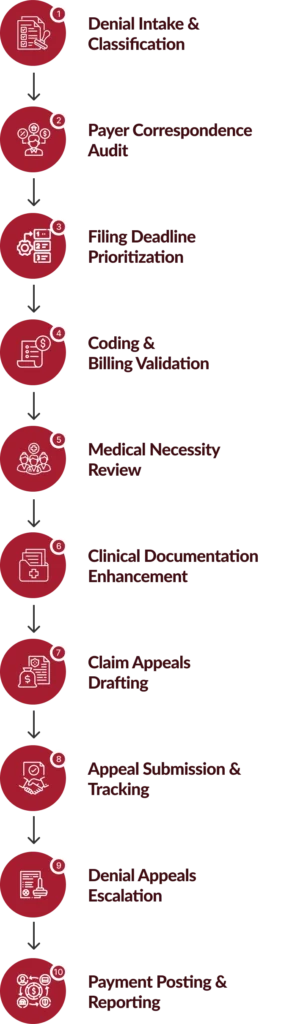
Benefits of Expert Correspondence & Claim Appeals
By aligning claim appeals workflows with clinical documentation and payer communication, we improve overturn rates and accelerate reimbursement.

Accelerated workflows and dedicated follow-ups shorten denial appeals cycles and improve reimbursement turnaround times.
Clinically supported documentation and coding validation enhance medical appeals success and payer acceptance.
Centralized payer correspondence management eliminates communication gaps and missed appeal deadlines.
Clinically validated medical appeals built on documentation, coding accuracy, and payer policy alignment.
Proactive denial appeals intervention recovers revenue that would otherwise be written off.
Flexible claim appeals support adapts to denial volume fluctuations without adding internal burden.
Results Driven by Appeals & Correspondence Expertise
Our claim appeals, denial appeals, and payer correspondence strategies deliver measurable gains in overturn rates, reimbursement speed, and revenue recovery.
Connected Appeals Workflows Using Existing Your EHR
Our teams operate directly within your EHR to manage claim appeals, payer correspondence, and medical appeals without disrupting workflows.
How EHR Alignment Helps:
- Faster documentation access for medical appeals
- Streamlined payer correspondence workflows
- Stronger claim appeals accuracy








Who we serve
Supporting healthcare organizations with specialized claim appeals, denial appeals, payer correspondence, and medical appeals services that strengthen reimbursement outcomes and denial recovery performance.

Hospitals
Supporting real-time claim appeals and payer correspondence across inpatient and outpatient encounters to reduce reimbursement delays and denial escalations.

Community & Integrated Health Systems
Delivering scalable denial appeals and medical appeals management across facilities to standardize workflows and strengthen enterprise-wide recovery performance.

Academic Medical Centers
Addressing complex documentation environments with clinically supported medical appeals and structured payer correspondence processes.

Medical Groups
Improving encounter-level reimbursement through efficient claim appeals and denial appeals resolution without disrupting coding workflows.

ACOs & Risk-Bearing Organizations
Enabling accurate reimbursement through coordinated medical appeals and payer correspondence aligned to value-based care models.
Client Experiences That Speak
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Optimize reimbursement through expert-led appeals support
Whether you’re managing rising denial volumes or complex payer correspondence, our specialists help streamline claim appeals and medical appeals to accelerate reimbursement outcomes.
Contact Form
Got Questions?
We’ve Got Answers!
Claim appeals services involve reviewing denied or underpaid claims, identifying the root cause, preparing supporting documentation, and submitting formal appeals to payers to recover rightful reimbursement.
Denial appeals address payer denials caused by coding errors, medical necessity disputes, authorization gaps, or documentation issues. A structured denial appeals process increases overturn rates and reduces revenue write-offs.
Payer correspondence management covers handling all communication with insurers — including denial letters, documentation requests, appeal notices, and follow-ups — to ensure timely responses and resolution.
Medical appeals focus specifically on clinical denials. They require physician documentation, medical necessity justification, and policy references to support why a service or procedure should be reimbursed.
Organizations often outsource when denial volumes rise, internal teams face bandwidth constraints, or specialized expertise is needed to manage complex claim appeals and payer correspondence efficiently.
With structured claim appeals and denial appeals workflows, providers typically see improved overturn rates, faster reimbursement cycles, reduced AR aging, and stronger financial performance.

























