Insurance Follow-Up Services for Accelerated Payer Reimbursements
Chirok Health’s insurance follow-up services deliver structured claims follow-up, proactive payer follow-up, and denial resolution workflows that keep reimbursements moving.

Insurance Follow-Up Challenges That Disrupt Revenue Goals
Gaps in insurance follow-up services cause escalating A/R days, inconsistent claims follow-up, and missed payer follow-up, ultimately delaying payments and impacting cash flow.



What Makes Our Insurance Follow-Up Services Operationally Strong?
Chirok Health combines structured insurance follow-up services with analytics-driven workflows to accelerate claim resolutions.
Revenue Recovery Differentiators:
- Faster insurance claim follow-up reduces reimbursement cycle times.
- Proactive payer follow-up prevents denial aging.
- Structured A/R follow-up improves cash acceleration.

Multi-Specialty Follow-Up Teams
Dedicated experts aligned to payer rules and specialty billing nuances.

Denial & Underpayment Recovery
Focused workflows to reopen, rework, and recover complex claims.

Insurance Follow-Up Services for FFS & Value-Based Care Models
Specialized insurance follow-up services aligned to fee-for-service volume and value-based reimbursement complexity.

Fee-For-Service Insurance Follow-Up
End-to-end insurance claim follow-up for high-volume billing environments, ensuring faster adjudication and reduced A/R days.

VBC Insurance Follow-Up
Insurance follow-up services aligned to bundled payments, shared savings, and quality-linked reimbursements.
Core Capabilities of Our Insurance Follow-Up Services
Our insurance follow-up services combine technology, payer expertise, and structured workflows to resolve claims faster and reduce A/R risk.

Denial Management & Appeals
Comprehensive insurance claim follow-up to investigate, correct, and appeal denied claims.

Payer Follow-Up & Communication
Direct payer follow-up via portals, calls, and escalations to move claims toward payment.

A/R Follow-Up & Aging Reduction
Insurance follow-up services designed to reduce AR days and unlock stuck revenue.

Contract Variance Resolution
Payer follow-up aligned to contract terms and fee schedule validation.
How Our Insurance Follow-Up Services Operate?
Our insurance follow-up services follow a defined lifecycle to track, resolve, and recover every claim.
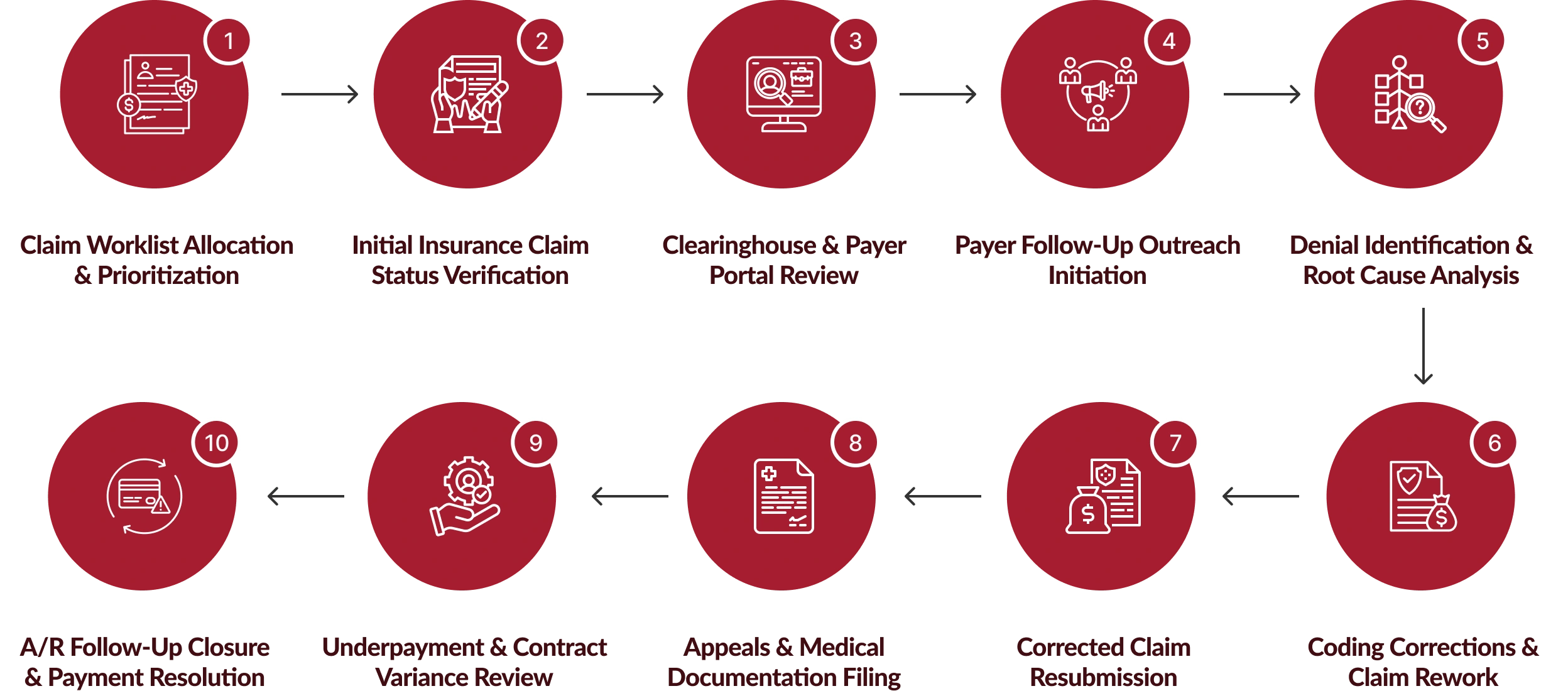
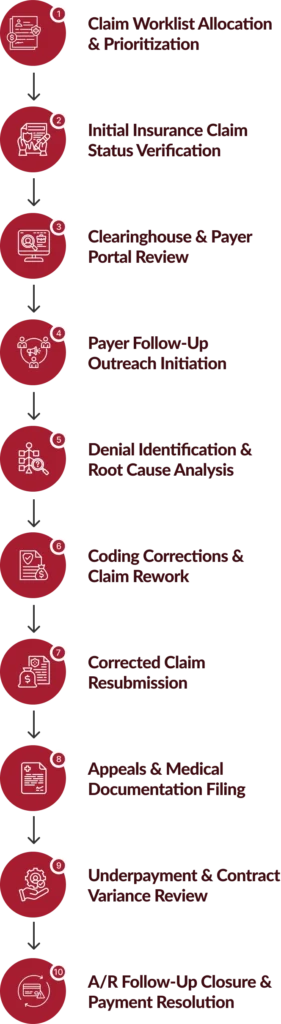
Operational & Revenue Benefits of Our Insurance Follow-Up Services
Our insurance follow-up services are designed to accelerate reimbursements, reduce A/R risk, and strengthen payer accountability.

Our insurance follow-up services streamline payer communications and eliminate claim stagnation, ensuring faster adjudication and predictable cash flow.
Structured A/R follow-up prioritizes high-value and aged claims, preventing revenue from slipping into write-off risk.
Dedicated claims follow-up workflows reopen, rework, and resolve denied claims within timely filing limits.
Consistent payer follow-up enforces response timelines and reduces unnecessary payment delays.
Insurance claim follow-up reporting provides transparency into claim status, payer trends, and recovery performance.
Measured Outcomes from Our Insurance Follow-Up Services
Our insurance follow-up services deliver measurable gains across reimbursement speed, denial recovery, and A/R reduction. Through structured claims follow-up and proactive payer follow-up, we help healthcare organizations unlock consistent revenue performance.
Insurance Follow-Up Expertise Across Leading EHR Platforms
By aligning our claims follow-up teams with your EHRs, we accelerate reimbursement workflows while maintaining data integrity.
Why EHR Expertise Matters?
- Real-time access strengthens insurance claim follow-up accuracy.
- Embedded workflows accelerate payer follow-up actions.
- Unified data improves A/R follow-up visibility.








Who we serve
Supporting healthcare organizations with specialized insurance follow-up services that reduce reimbursement delays, strengthen payer follow-up performance, and improve clean claims outcomes across complex billing environments.

Hospitals
Enabling real-time insurance claim follow-up across inpatient and outpatient encounters to minimize payment delays and prevent revenue leakage.

Community & Integrated Health Systems
Delivering scalable claims follow-up and payer follow-up workflows that standardize reimbursement recovery across multi-facility networks.

Academic Medical Centers
Managing complex billing structures through structured insurance follow-up services that address documentation gaps and payer requirements.

Medical Groups
Strengthening encounter-level reimbursement through proactive A/R follow-up and denial resolution workflows.

ACOs & Risk-Bearing Organizations
Supporting value-based reimbursement through coordinated payer follow-up and insurance claim follow-up strategies.
Client Stories on Our Insurance Follow-Up Services
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Let’s Optimize Your Claims Follow-Up Outcomes
Our specialists work as an extension of your revenue cycle team, handling claims follow-up, payer follow-up, and denial recovery with precision. Share your requirements to get started.
Contact Form
Got Questions?
We’ve Got Answers!
Insurance follow-up services involve tracking, investigating, and resolving unpaid or underpaid claims with payers after submission. This includes claims follow-up, denial resolution, payer communication, and A/R follow-up to ensure providers receive accurate and timely reimbursements.
Insurance follow-up services help reduce payment delays, recover denied claims, and prevent revenue leakage. Without consistent insurance claim follow-up and payer follow-up, unresolved claims can age beyond filing limits and negatively impact cash flow.
The insurance claim follow-up process typically includes claim status checks, payer follow-up calls, denial analysis, corrected claim resubmissions, appeals filing, underpayment reviews, and A/R follow-up until payment resolution is completed.
Through structured A/R follow-up workflows, high-value and aged claims are prioritized for immediate action. Regular payer follow-up and escalation protocols accelerate adjudication, reducing overall accounts receivable aging.
Claims follow-up teams manage administrative, coding, authorization, medical necessity, and timely filing denials. Insurance follow-up services investigate root causes, submit corrections, and pursue appeals to recover reimbursements.
Yes. Most insurance follow-up services integrate directly with EHRs and practice management systems to access claim data, documentation, and payer communications, enabling more efficient claims follow-up and reporting.





















