Credit Balance Management for Healthcare Organizations
Optimize financial accuracy and compliance with proactive credit balance management. Our experts identify overpayments, validate liabilities, and execute timely refunds through structured RCM credit balance services.

Credit Balance Management Challenges in Healthcare Organizations
Without structured credit balance management, organizations face refund delays, compliance exposure, and missed overpayment recovery services opportunities.



Why Chirok Health’s Credit Balance Management Works?
Chirok Health combines analytics, payer intelligence, and workflow automation to streamline credit balance management, accelerate overpayment recovery services, and ensure refund compliance across complex RCM environments.
The Revenue Protection Difference
- Improves visibility into enterprise credit positions
- Minimizes revenue leakage from unresolved overpayments
- Optimizes patient credit balance services workflows

Advanced Credit Analytics
AI-assisted credit identification and liability classification.

Payer Refund Expertise
Specialized workflows for complex payer refund regulations.

Credit Balance Management Across FFS & VBC Models
Chirok Health aligns credit workflows to reimbursement structures, reducing exposure and accelerating RCM credit balance services performance.

FFS Credit Balance Resolution
Structured audits detect aged credits and accelerate overpayment recovery services within transactional reimbursement models.
VBC Credit Balance Resolution
We validate attribution, reconcile incentive payments, and manage refunds across value-based reimbursement models.
Core Capabilities of Our Credit Balance Management Services
Our credit balance management framework combines analytics, payer research, and compliance workflows to accelerate overpayment recovery services and streamline refund resolution.

Credit Discovery Analysis
Audits uncover payer and patient credit balances across billing systems, preventing aged balances and missed recovery opportunities.

Liability Validation
We validate payer vs patient responsibility through remittance reviews, COB analysis, and contract verification.

Payer Refund Management
Our team executes compliant overpayment recovery services, managing payer communications and refund processing.

Patient Balance Management
Dedicated patient credit balance services manage statements, communications, and timely refund issuance.
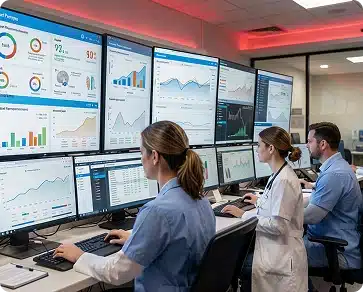
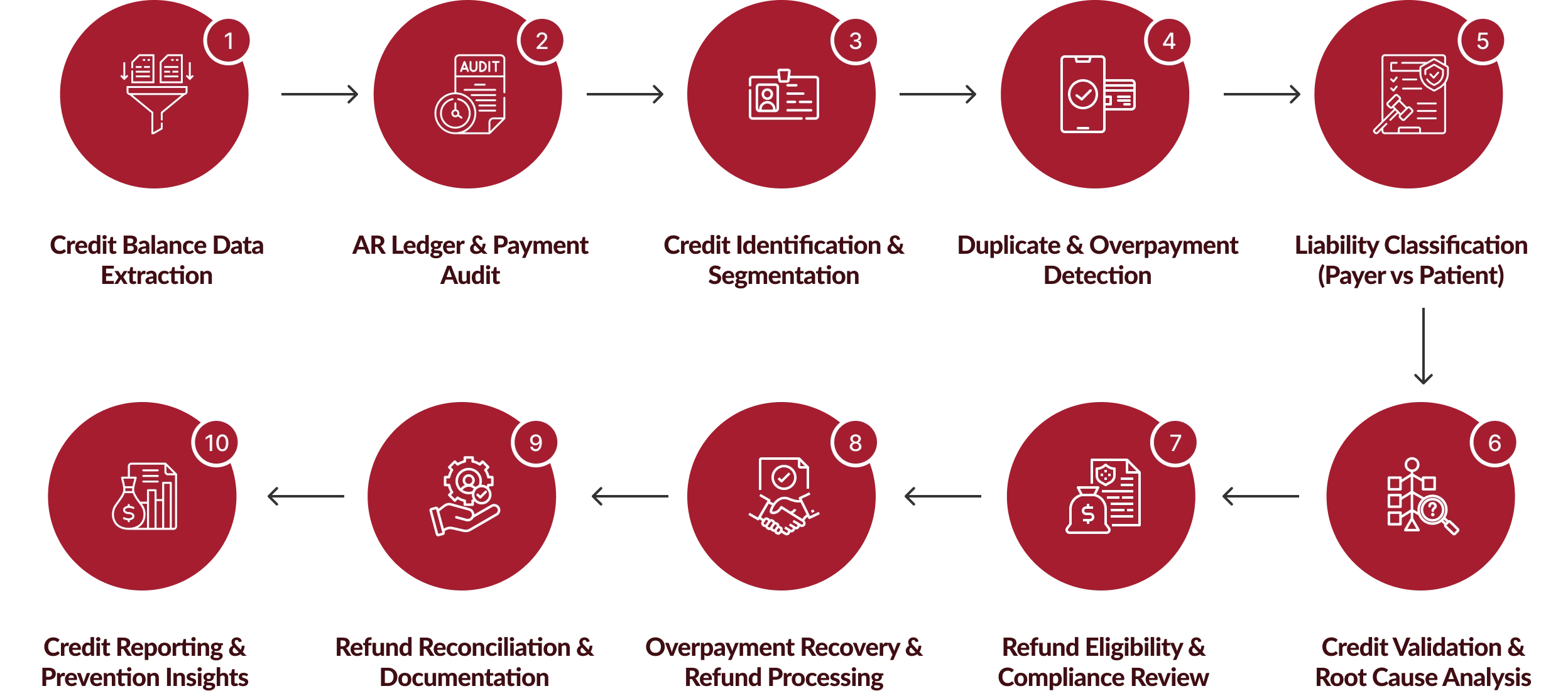
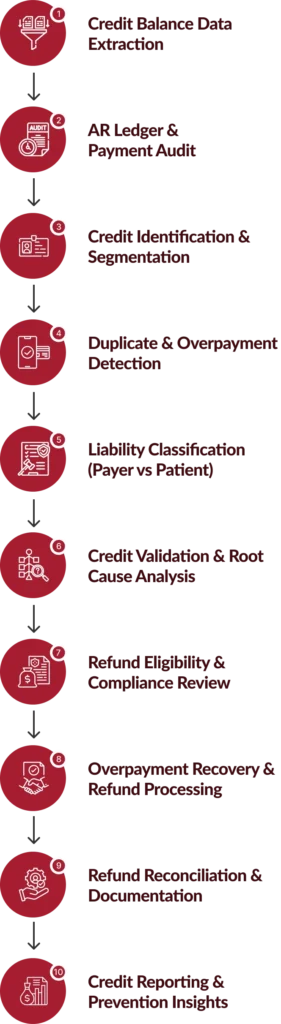
Our Credit Balance Management Process Workflow
We follow a standardized resolution framework designed to streamline investigations, reduce refund delays, and optimize enterprise-wide RCM credit balance services performance.
Benefits of Our Credit Balance Management Services
We deliver measurable financial and operational improvements through structured overpayment recovery services and patient credit resolution workflows.

Streamlined investigations and automation reduce aging credits and improve turnaround time across payer and patient credit balance services workflows.
Accurate credit tracking enhances financial reporting and frees tied-up revenue from unresolved overpayments.
Built-in controls ensure timely refunds and adherence to payer, CMS, and audit requirements.
Proactive identification prevents write-offs and captures recoverable dollars through structured overpayment recovery services.
Transparent refund communication improves trust, satisfaction, and patient loyalty.
Performance Outcomes Credit Balance Management
Our data-driven credit balance management model delivers measurable financial recovery, accelerates overpayment recovery services, and strengthens compliance across enterprise RCM operations.
Deep EHR Expertise in our Credit Balance Management
We operate within your EHR to streamline data access, accelerate overpayment recovery services, and strengthen refund compliance.
EHR Expertise Benefits
- Improves accuracy in patient credit balance services
- Reduces manual reconciliation efforts
- Strengthens audit-ready documentation trails








Who we serve
We partner with providers and healthcare networks to deliver scalable overpayment recovery services and compliant patient credit balance services operations.

Hospitals
Managing high-volume payer and patient credits across inpatient and outpatient services to accelerate refunds and reduce aged AR exposure.

Community & Integrated Health Systemss
Standardizing enterprise-wide RCM credit balance services workflows to improve visibility, compliance, and refund performance across facilities.

Academic Medical Centers
Resolving credits within complex billing, teaching physician, and multi-entity reimbursement structures.

Medical Groups
Improving encounter-level credit resolution through streamlined investigations and faster patient credit balance services processing.

ACOs & Risk-Bearing Organizations
Addressing overpayments tied to bundled payments, shared savings, and attribution models within value-based care contracts.
Trusted Voices from Our Clients
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Partner with Experts in Credit Balance Management
Speak with our specialists to explore structured overpayment recovery services designed for your reimbursement model, scale, and operational complexity.
Contact Form
Got Questions?
We’ve Got Answers!
Strategic credit balance management improves net revenue accuracy by recovering overpayments, reducing aged credits, and freeing tied-up cash. It also strengthens financial reporting integrity and minimizes avoidable write-offs across the revenue cycle.
Decision makers should evaluate domain expertise, refund compliance processes, payer follow-up capabilities, reporting transparency, and scalability. Mature credit balance resolution services partners also provide audit trails and root-cause analytics to prevent recurring credits.
Outsourced overpayment recovery services handle credit audits, payer communication, refund processing, and documentation management. This reduces internal workload while accelerating resolution timelines and improving recovery yield.
Structured RCM credit balance services ensure timely refunds aligned with CMS and payer requirements. They maintain documentation, approval workflows, and audit logs to reduce regulatory exposure and penalty risk.
Yes. Enterprise-grade credit balance management programs standardize workflows across hospitals, medical groups, and outpatient entities, delivering centralized visibility and consistent refund governance.
Optimized patient credit balance services reduce refund backlogs, improve patient financial experience, and lower call center escalations. Financially, organizations benefit from operational cost savings and improved brand trust.

























