End Revenue Delays with Accurate Payment Posting Services
From automated ERA posting services to detailed EOB processing services, we ensure every payment, adjustment, and denial code is posted accurately to accelerate downstream AR workflows and financial reporting.

Payment Posting Challenges That Disrupt Revenue Accuracy
Manual workflows, remittance complexity, and reconciliation gaps often slow AR resolution and obscure true financial performance.



What Makes Our Payment Posting Services Operationally Superior?
Chirok Health combines automation, remittance intelligence, and payer-specific expertise to eliminate posting errors and accelerate reconciliation timelines.
What Set Us Apart
- Auto-validated ERA posting services reduce manual intervention and posting lag.
- Structured EOB processing services accelerate denial identification.
- Scalable medical payment posting services support high-volume growth without backlog risk.

Remittance Automation Specialists
Advanced workflows streamline payer files, adjustments, and variance detection at scale.

Multi-Specialty Posting Expertise
Supporting diverse billing models across physician, facility, and outpatient environments.

Payment Posting Services for FFS and Value-Based Care Models
Chirok Health adapts posting logic, reconciliation rules, and adjustment mapping to support diverse payer contracts across FFS and value-based reimbursement environments.

Fee-For-Service Payment Posting
Our medical payment posting services ensure precise allocation of service-based reimbursements and denial codes.
Value-Based Care Payment Posting
Our RCM payment posting services track value-linked incentives, risk adjustments, and care quality payouts.
Core Capabilities of Our Payment Posting Services
Chirok Health’s RCM payment posting services integrate technology and human validation to manage high-volume payer and patient payments without delays.

Electronic Remittance Posting
Our ERA posting services streamline electronic payment imports and reconciliation workflows.

EOB Posting Solutions
Our EOB processing services eliminate manual backlog and accelerate secondary billing.

Patient Payment Posting
Posting copays, deductibles, and online payments with real-time account reconciliation.

Underpayment Identification
Our medical payment posting services detect underpayments and payer variances.
How Our Medical Payment Posting Services Operate?
Chirok Health standardizes posting operations across payers, payment formats, and reimbursement models to eliminate variance and backlog risk.
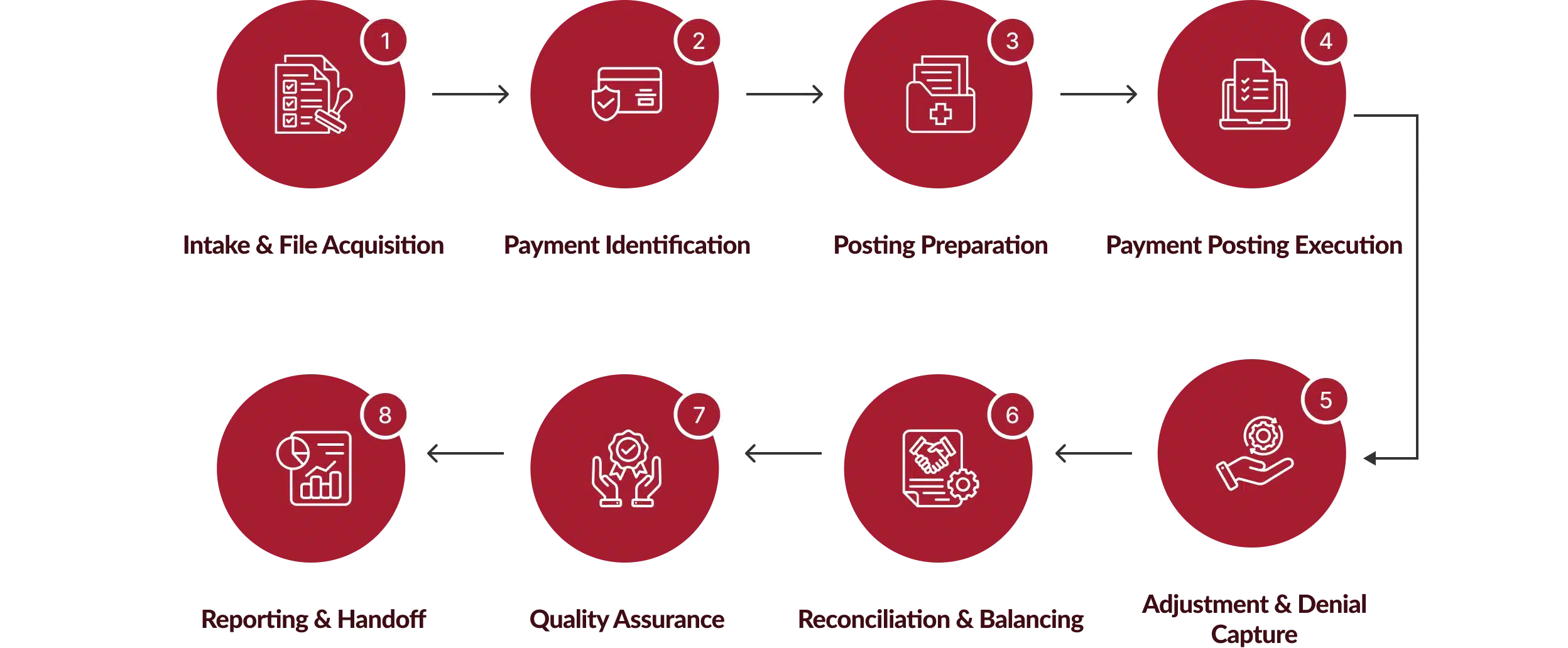
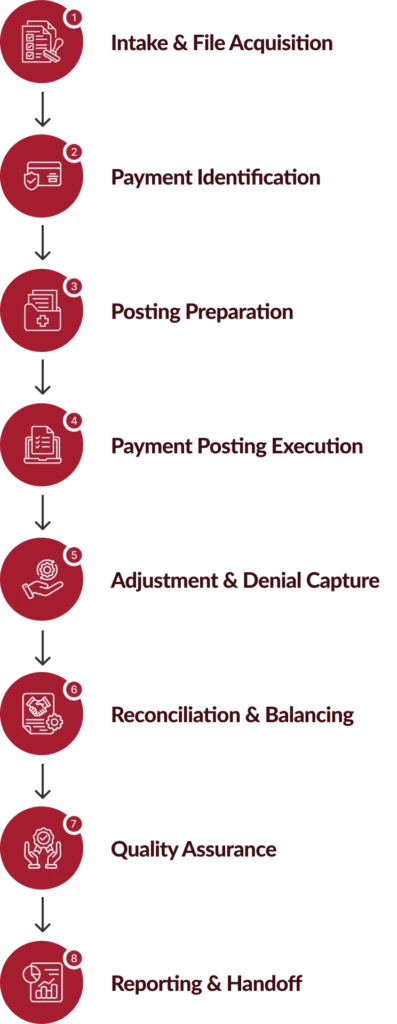
Benefits of Outsourcing Payment Posting Services
Our payment posting services go beyond transaction entry; they strengthen reconciliation accuracy, accelerate AR movement, and improve financial visibility across the revenue cycle.

Structured EOB processing services capture denial codes early, enabling faster appeals and corrections.
We validate payer reimbursements against contracted rates to detect underpayments and variances.
Our RCM payment posting services adapt to transaction surges without compromising turnaround time.
Accurate posting improves net collection metrics, payer performance tracking, and revenue forecasting.
Outsourcing medical payment posting services frees internal teams to focus on AR resolution and patient engagement.
Performance Metrics That Define Our Posting Excellence
Chirok Health delivers consistent, audit-ready posting performance across high-volume reimbursement environments. Our payment posting services improve reconciliation speed, reduce unapplied cash, and strengthen revenue reporting accuracy.
Payment Posting Services Using Leading EHR Platforms
Our teams are trained across multi-specialty EHRs, enabling faster remittance processing without workflow disruption.
Advantages of EHR-Aligned Posting
- System-native posting eliminates data synchronization errors.
- Embedded workflows accelerate ERA and EOB processing timelines.
- Real-time reconciliation strengthens financial reporting accuracy.








Who we serve
Chirok Health supports healthcare organizations with specialized payment posting services that accelerate remittance processing, reduce unapplied cash, and strengthen clean revenue reconciliation across payer and patient payment workflows.

Hospitals
Supporting high-volume remittance posting across inpatient and outpatient services to reduce reconciliation delays and improve cash flow visibility.

Community & Integrated Health Systemss
Delivering scalable medical payment posting services that standardize reconciliation workflows across multi-facility networks.

Academic Medical Centers
Managing complex payer structures, teaching physician billing, and grant-linked reimbursements with structured posting accuracy.

Medical Groups
Improving encounter-level payment allocation and adjustment posting without disrupting coding or billing operations.

ACOs & Risk-Bearing Organizations
Aligning posting workflows to bundled payments, shared savings, and risk-adjusted reimbursement models.
Experiences Shared by Our Clients
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Let’s Optimize Your Payment Posting Operations
Whether you manage a physician group, hospital system, or billing enterprise, Chirok Health’s payment posting services are designed to improve remittance turnaround, eliminate unapplied cash, and strengthen financial reporting accuracy.
Contact Form
Got Questions?
We’ve Got Answers!
Payment posting services involve recording payer and patient payments into the billing system and reconciling them against submitted claims. This includes posting ERAs, reviewing EOBs, applying adjustments, and identifying denials to maintain accurate accounts receivable and financial reporting.
Outsourced medical payment posting services typically cover ERA auto-posting, manual EOB posting, patient payment allocation, denial code capture, contractual adjustment posting, and deposit reconciliation. Many providers also include QA audits and variance reporting.
ERA posting services automate the import and posting of electronic remittance files, reducing manual data entry, minimizing errors, and accelerating cash application. This speeds up secondary billing, denial follow-ups, and overall AR resolution timelines.
While ERAs handle electronic payments, many payers still issue paper remittances. EOB processing services ensure these payments are accurately reviewed, digitized, and posted, preventing posting gaps, unapplied cash, and reconciliation discrepancies.
RCM payment posting services directly influence key metrics such as posting turnaround time, unapplied cash rate, denial identification speed, net collection rate, and AR days. Accurate posting also improves payer performance analysis and revenue forecasting.
Accurate posting captures denial codes, adjustment reasons, and payer variances at the transaction level. This visibility enables faster appeals, underpayment recovery, and root-cause analysis to prevent recurring reimbursement issues.

























