Ancillary Medical Coding Services for Outpatient and Diagnostic Care
Chirok Health delivers specialized ancillary services medical coding across outpatient and facility settings. Our certified ancillary coders ensure compliant, audit-ready coding for labs, radiology, therapies, and diagnostic services, without revenue leakage.

Coding Challenges That Emerge as Inpatient and Outpatient Volumes Grow
Ancillary medical coding is uniquely vulnerable to errors because it spans diagnostics, therapies, and technical components that rely on fragmented documentation.



What Makes Chirok Health’s Ancillary Coding Consistently Accurate?
Our model aligns documentation review, coding precision, and compliance validation before claims ever reach billing.
Why We Are Reliable?
- Coding aligned to physician orders and interpretations.
- Accurate units, modifiers, and components.
- Payer rules and NCCI edits applied upfront.

AHIMA / AAPC / ACDIS Certified Coders
Certified expertise across ancillary coding workflows

Specialty-Focused Ancillary Coding
Coding aligned to outpatient diagnostic services

Ancillary Coding Services Across Fee-for-Service and Value-Based Care
Accurate reimbursement in fee-for-service models while strengthening data integrity and risk capture in value-based care.

Fee-for-Service Reimbursement Accuracy
Accurate ancillary coding that protects units, modifiers, and payment integrity

Value-Based Care Data Alignment
Ancillary coding that strengthens quality reporting and risk adjustment models
Core Components of Ancillary Medical Coding Services
Ancillary medical coding services require precision across diagnostics, therapies, and technical components. We ensure accuracy, compliance, and consistency across outpatient and facility billing.

Order & Documentation Validation
Clinical orders, reports, and encounter documentation reviewed to support ancillary services medical coding and medical necessity.

Outpatient Ancillary Code Assignment
Accurate CPT and HCPCS assignment for outpatient ancillary coding, including units, modifiers, and component logic.

Modifier & Bundling Integrity
Proper application of modifiers and NCCI edits to prevent bundling errors, underpayments, and downstream denials.

Payer & Compliance Alignment
Ancillary medical coders align coding with payer rules, LCDs, and audit thresholds across services and settings.
How Our Ancillary Coding Services Work?
Chirok Health’s ancillary medical coding services follow a structured, review-driven workflow that aligns documentation, coding logic, and compliance checks before claims submission.
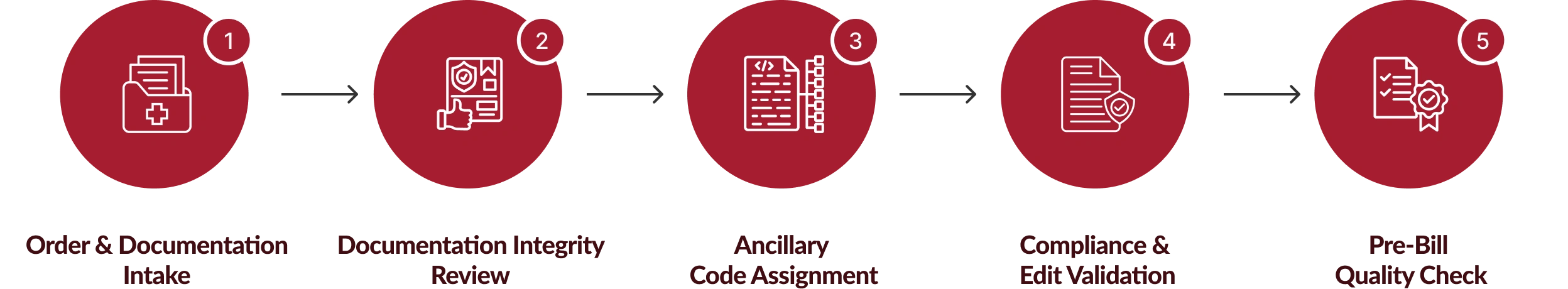

What Benefits Can Organizations Expect from Our Ancillary Coding Services?

Accurate ancillary medical coding services ensure billable diagnostic, therapy, and technical services are fully captured, reducing undercoding and preventing avoidable revenue loss across outpatient encounters.
Well-structured ancillary services medical coding minimizes documentation gaps, modifier errors, and bundling issues, leading to fewer payer denials and significantly less rework for billing teams.
Ancillary medical coders apply payer rules, LCDs, and NCCI edits consistently, helping organizations remain audit-ready while reducing exposure to recoupments and retrospective compliance risk.
Standardized outpatient ancillary coding workflows reduce manual intervention, speed up coding turnaround times, and allow internal teams to scale operations without sacrificing accuracy.
High-quality ancillary coding improves data integrity used for quality reporting, utilization analysis, and risk adjustment, supporting more accurate performance measurement under value-based care programs.
Performance Metrics That Reflect Real Ancillary Coding Outcomes
Chirok Health’s ancillary medical coding services are measured by operational accuracy, financial impact, and compliance performance, tracked consistently across outpatient and facility environments.
Ancillary Coding Services that Adapt to Your Existing EHR
Our coders operate directly within your EHR without disrupting established workflows.
Why EHR Adaptability is Efficient?
- Faster onboarding with minimal system changes
- Reduced workflow friction for clinical and coding teams
- Cleaner, system-native data for reporting and audits








Who We Serve?
Chirok Health supports healthcare organizations that rely on accurate ancillary coding to protect reimbursement, strengthen compliance, and maintain operational control across diverse care settings.

Hospitals & Health Systems
Supporting accurate inpatient medical coding and outpatient medical coding to improve DRG integrity, APC assignment, and audit readiness at scale.

Outpatient Care Organizations
Delivering consistent outpatient coding across clinics, EDs, and ambulatory settings without compromising accuracy or turnaround time.

Academic Medical Centers
Managing complex, high-acuity inpatient and outpatient encounters with clinically validated coding that supports teaching environments and compliance.

Medical Groups & Physician Practices
Improving documentation alignment and code accuracy across specialties to support compliant billing and reliable revenue performance.

ACOs & Risk-Bearing Organizations
Ensuring accurate inpatient and outpatient code capture to support quality reporting, financial performance, and value-based contract requirements.
Value-Based Care RCM Staff Augmentation
Dedicated Chirok Health specialists extend your value-based care revenue cycle, supporting risk, quality, and contract performance across your organization.
Hear from Organizations We’ve Helped
Chirok Health’s partnership has been invaluable, demonstrating remarkable adaptability in meeting our needs. Their comprehensive chart reviews ensure chronic conditions and potential health conditions are brought forth to our providers on time, enabling us to establish tailored care plans that truly meet our patients' needs.
Chief Financial Officer

Our Chirok partnership over the years has been amazing. The depth of knowledge and expertise is a given for Chirok, but their dedication to getting things right, working with us to improve each day, and the warmth of their people has set them apart. They are close colleagues and friends as well as coding partners, and we are very grateful for that.
Medical Compliance Officer

The Chirok team consistently puts quality at the forefront, maintaining an unwavering dedication to compliance. Their commitment to accuracy is unparalleled, ensuring that our organization benefits from the highest standards without compromise. They are prompt, supportive, and a joy to work with. We are grateful for a partnership that blends excellence with efficiency.
Chief Operations Officer, Ambulatory Services

Get in Touch
Let’s improve accuracy, compliance, and reimbursement outcomes.
Whether you manage outpatient diagnostics, therapies, or complex ancillary workflows, Chirok Health helps organizations strengthen ancillary medical coding accuracy, reduce denials, and scale confidently across care settings.
Contact Form
FAQs
We have got answers!
Chirok Health improves reimbursement accuracy by validating orders, documentation, units, modifiers, and technical components before billing. This prevents undercoding, missed ancillary services, and bundling errors that commonly reduce outpatient revenue.
Yes. Chirok Health reduces ancillary-related denials by applying payer rules, LCDs, and NCCI edits upfront, ensuring claims are supported, compliant, and clean before submission.
Revenue leakage often occurs due to missing add-on codes, incorrect units, unsupported modifiers, and improperly bundled diagnostic services. Chirok Health addresses these gaps through specialty-focused ancillary coding review.
Chirok Health aligns ancillary coding to physician orders, clinical documentation, payer policies, and NCCI edits, supported by pre-bill quality checks that reduce audit exposure and recoupment risk.
Yes. Chirok Health’s ancillary coders are AAPC- and AHIMA-certified and trained specifically in outpatient diagnostic, laboratory, radiology, and therapy coding workflows.
Chirok Health applies modifier logic based on documentation support for professional and technical components, distinct services, and payer-specific rules to prevent underpayments and denials.
Yes. Chirok Health delivers ancillary coding services directly within your existing EHR, enabling faster onboarding, minimal workflow disruption, and system-native audit trails.
Our standardized workflows, specialty-aligned coders, and quality controls allow Chirok Health to scale ancillary coding services efficiently as outpatient and diagnostic volumes increase.
Turnaround times depend on volume and complexity, but Chirok Health’s structured ancillary coding workflows are designed to support timely coding without sacrificing accuracy or compliance.
Accurate ancillary coding from Chirok Health improves the reliability of diagnostic and utilization data used in quality reporting, cost analysis, and performance measurement under value-based care models.
Yes. Inaccurate ancillary coding can distort utilization trends and quality metrics. Chirok Health ensures ancillary data integrity to support reliable reporting and informed decision-making.
Chirok Health combines certified ancillary coders, payer-aligned compliance checks, EHR adaptability, and measurable performance outcomes to deliver audit-ready coding at scale.
Most organizations can begin onboarding quickly once access, workflows, and documentation standards are defined. Chirok Health supports a structured onboarding process to ensure a smooth transition.
Yes. Chirok Health supports hospitals, health systems, outpatient clinics, imaging centers, physician groups, and risk-bearing organizations with tailored ancillary coding solutions.

























