Retrospective Review Services That Protect Payment Integrity and Reduce Risk
Chirok Health delivers payer-focused retrospective clinical audits that validate documentation accuracy, medical necessity, and coding compliance, helping health plans identify overpayments, reduce audit risk, and strengthen regulatory confidence.

Operational Challenges in Scaling Retrospective Reviews
As retrospective audits expand across claims and contracts, healthcare payors face rising complexity, operational strain, and compliance risk.



What is Different About Our Retrospective Review Services?
Chirok Health applies clinically rigorous, payer-aligned retrospective reviews that prioritize accuracy, consistency, and defensibility, helping health plans scale audit programs with confidence.
Why It Matters for Healthcare Payors?
- Evidence-based retrospective clinical audits aligned to payer policy and coding standards.
- High-volume retrospective audits delivered with consistent accuracy and turnaround.
- Retrospective review insurance programs tailored to each health plan’s policies and risk models.

Certified Clinical & Coding Experts
Reviews conducted by experts with deep payer-side experience.

Multi-Specialty Review
Supporting retrospective audit programs across various specialties.

Retrospective Review Services Aligned to Payment Models
Purpose-built retrospective audits that support both value-based care and fee-for-service payment integrity strategies.

Value-Based Care Reviews
Retrospective clinical audits validate risk-adjusted diagnoses, care documentation, and coding accuracy to support compliant reimbursement in value-based care programs.

Fee-for-Service Reviews
Targeted retrospective audits assess medical necessity, coding accuracy, and payment compliance to identify overpayments and reduce downstream audit risk.
Retrospective Review Services Core Capabilities for Healthcare Payors
Chirok Health’s retrospective review services combine clinical, coding, and compliance audits to protect payment integrity and reduce risk.

Clinical Documentation Review
Retrospective clinical audits assess whether documentation fully supports reported diagnoses, conditions, and services in alignment with payer policy and clinical guidelines.

Coding Accuracy Validation
Retrospective audits validate ICD-10, CPT, and DRG assignment accuracy to identify unsupported coding and potential overpayment exposure.

Medical Necessity Audits
Structured retrospective audits evaluate medical necessity against payer coverage criteria, CMS guidance, and evidence-based standards.

Compliance & Appeals Support
Audit findings are documented with defensible rationale to support appeals, regulatory review, and audit transparency.
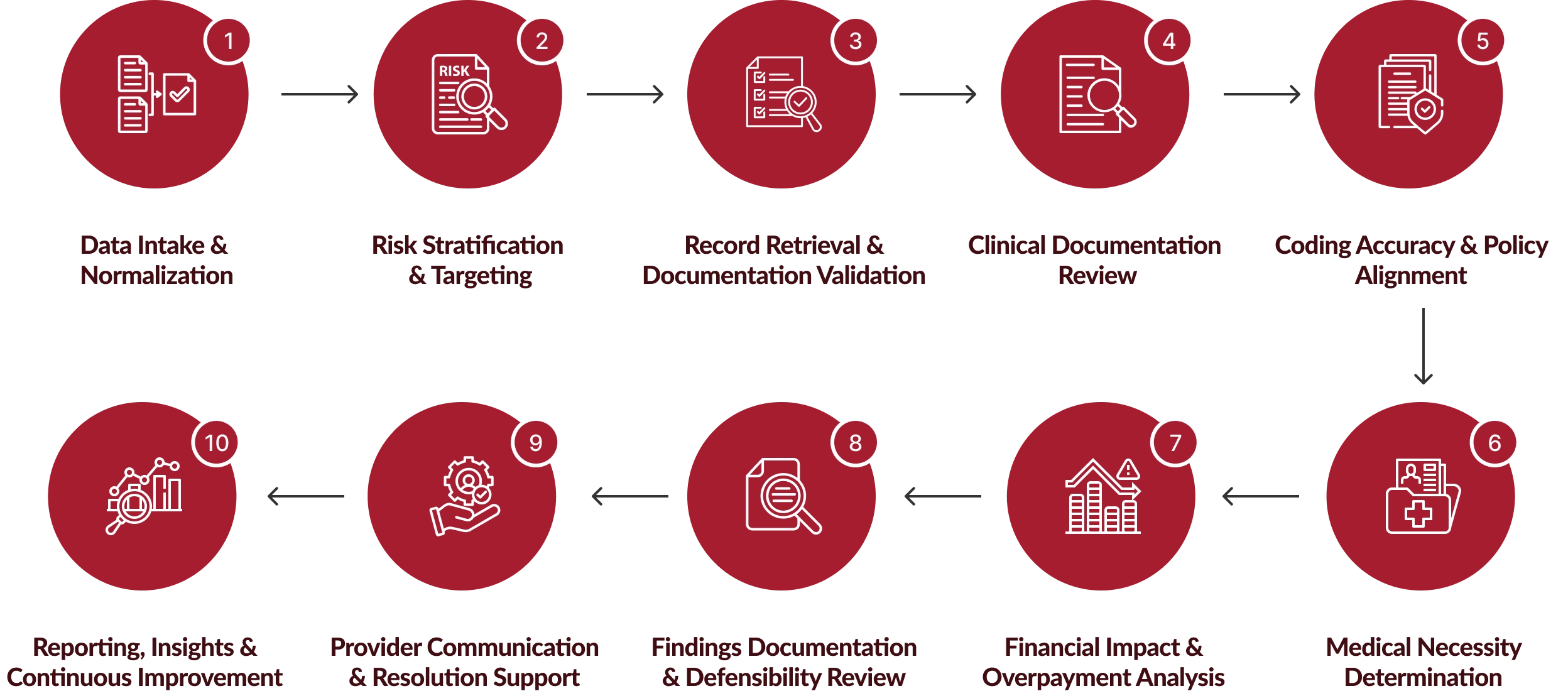
How Retrospective Review Services Work for Healthcare Payors?
Chirok Health follows a structured, payer-aligned retrospective review workflow designed to ensure accuracy, defensibility, and consistent outcomes across claims, contracts, and care models.

Undeniable Benefits of Retrospective Review Services for Payors
Retrospective review programs are designed to strengthen payment integrity, audit defensibility, and operational efficiency across health plans.

Retrospective clinical audits identify unsupported payments, validate reimbursement accuracy, and reduce financial leakage across claims, contracts, and care models.
Defensible retrospective audit findings withstand appeals and regulatory scrutiny.
Systematic reviews improve alignment between clinical documentation and reported codes
Structured workflows support high-volume retrospective audits without overburdening internal teams.
Clear, evidence-based findings support more productive audit resolution discussions.
Proven Retrospective Review Outcomes for Healthcare Payors
Chirok Health’s retrospective review services deliver measurable improvements across payment integrity, risk adjustment accuracy, and audit performance, supported by consistent, real-world results.
New HCC Improvement
Net New HCC Per Patient
RAF Improvement
Gap Closure Improvement
Net New Closures per Member
Priority Measure Rate Lift / Stars Movement
Get in Touch
Start a conversation about Retrospective Review
Chirok Health works with healthcare payors to strengthen payment integrity, improve audit defensibility, and scale retrospective review programs with confidence. Connect with our team to discuss your specific review goals.
Contact Form
Got Questions?
We’ve Got Answers!
Why do payers need retrospective reviews today?
As regulatory scrutiny increases, retrospective reviews help organizations validate previously submitted diagnoses, identify missed or unsupported risk conditions, and ensure accurate reimbursement without increasing audit exposure.
How does Chirok Health’s retrospective review support value-based care programs?
Our retrospective reviews are designed to strengthen risk adjustment accuracy and compliance, ensuring patient complexity is fully and defensibly captured across value-based contracts.
Is this service focused on revenue recovery or compliance?
Both. Chirok Health balances legitimate revenue identification with strict clinical and coding validation, ensuring every finding is compliant, defensible, and audit-ready.
How is Chirok Health’s retrospective review different from traditional HCC gap reviews?
Unlike volume-driven HCC reviews, Chirok Health applies clinical validation, AI-supported analytics, and compliance oversight to prevent overcoding, unsupported diagnoses, and future audit risk.
Can retrospective reviews increase RADV or OIG audit risk?
Only when done incorrectly. Chirok Health mitigates this risk through conservative review standards, documentation sufficiency checks, and compliance governance aligned with CMS guidelines.
Which organizations benefit most from retrospective review services?
Retrospective reviews are most effective for payers, risk-bearing providers, ACOs, and large medical groups managing complex populations and multiple value-based contracts.
How does Chirok Health ensure findings are clinically supported?
All identified conditions undergo clinical validation and coding review, ensuring diagnoses are supported by documentation and meet CMS risk adjustment requirements.
Can this service be engaged independently from other Chirok Health offerings?
Yes. Retrospective review services can be engaged as a standalone engagement for auditing, monitoring, or performance assessment, without requiring broader RCM or CDI services.
How soon can organizations see measurable outcomes?
Most organizations begin seeing measurable improvements within 60–90 days, including improved risk capture visibility, reduced documentation gaps, and stronger compliance posture.
How do retrospective reviews support long-term risk adjustment improvement?
Beyond immediate findings, retrospective insights inform provider education, documentation standards, and governance models, helping organizations reduce future gaps and sustain performance.

























